Did you know your body’s energy production declines by 8% every decade after age 30? This startling fact highlights the critical role of mitochondrial health in your overall well-being. As you grow older, these tiny powerhouses in your cells become less efficient, impacting everything from metabolism to fat distribution.
Over time, oxidative stress and DNA mutations accumulate, accelerating cellular aging. This process not only reduces energy levels but also alters how your body stores fat. The good news? Lifestyle changes like regular exercise and a balanced diet can help counteract these effects.
Understanding these changes is the first step toward maintaining vitality as you age. Let’s explore how you can support your mitochondrial function and optimize your health.
Key Takeaways
- Energy production declines by 8% per decade after age 30.
- Oxidative stress and DNA mutations accelerate cellular aging.
- Fat storage patterns shift significantly with age.
- Exercise and diet can improve mitochondrial health.
- Human studies confirm these age-related metabolic changes.
Introduction to Mitochondria and Aging
Mitochondria are often called the powerhouses of your cells, but their role goes beyond energy production. These tiny structures are essential for maintaining your body’s energy balance and overall health. Understanding their function and how they change over time is key to supporting your well-being.
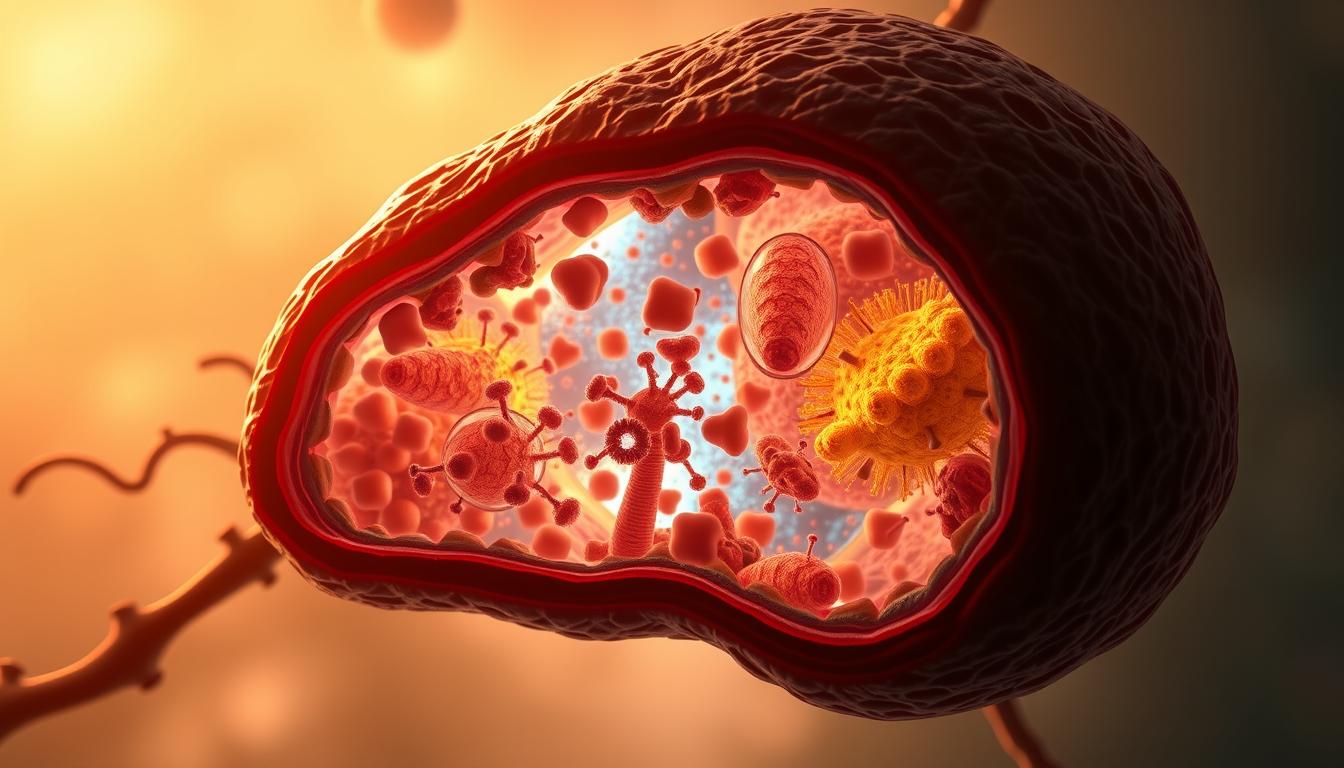
What Are Mitochondria?
Mitochondria are unique organelles with a double membrane and inner folds called cristae. They contain over 1,000 proteins, but only 13 are encoded by their own DNA. This structure allows them to efficiently produce energy through a process called oxidative phosphorylation (OXPHOS).
The Role of Mitochondria in Cellular Energy
Mitochondria generate about 90% of your cell’s energy in the form of ATP. This process occurs in the electron transport chain, a series of protein complexes (I-V) located in the inner membrane. As electrons move through these complexes, energy is released and used to produce ATP.
Why Aging Impacts Mitochondrial Function
As you age, the efficiency of mitochondrial energy production declines. Studies show that Complex I and III in the electron transport chain become 15-26% less efficient. Additionally, reactive oxygen species (ROS), which are byproducts of energy production, can damage mitochondrial DNA. This damage accumulates over time, further reducing function.
Research on 71-year-old subjects revealed a 26% lower VO2 max, a measure of oxygen utilization, compared to younger individuals. This highlights the significant impact of aging on mitochondrial health and energy production.
The Science of Aging: A Cellular Perspective
The science behind aging reveals profound changes in your cells over time. These transformations are not just superficial; they affect your body’s functionality at a fundamental level. By understanding these processes, you can take steps to support your health as you grow older.
Understanding the Aging Process
Aging is marked by both chronological and biological changes. Chronological aging refers to the passage of time, while biological aging reflects the wear and tear on your cells. One key marker of biological aging is telomere attrition, where the protective caps at the ends of your chromosomes shorten with each cell division. This process contributes to replicative senescence, where cells lose their ability to divide.
How Cells Change Over Time
As you age, your cells undergo significant alterations. For example, sarcopenia, the loss of muscle mass, is linked to mitochondrial apoptosis, where damaged cells self-destruct. Additionally, nuclear DNA repair becomes less efficient, leading to an accumulation of mutations. These changes can impair cellular function and contribute to age-related diseases.
The Role of DNA in Aging
DNA plays a critical role in the aging process. Research shows a 16-fold increase in oxidative damage markers, such as 8-OHdG, in the mitochondrial DNA of aged rats. This oxidative stress accelerates cellular aging and disrupts energy production. Protecting your DNA through lifestyle choices can help mitigate these effects.
| Hallmark of Aging | Description |
|---|---|
| Telomere Attrition | Shortening of chromosome ends, leading to cell senescence. |
| Mitochondrial Dysfunction | Decline in energy production efficiency. |
| DNA Repair Inefficiencies | Reduced ability to fix DNA damage. |
| Oxidative Stress | Accumulation of reactive oxygen species damaging cells. |
Mitochondrial Dysfunction: A Hallmark of Aging
Your body’s ability to produce energy diminishes as you grow older, largely due to changes in cellular function. One of the most significant factors in this decline is mitochondrial dysfunction. This condition disrupts the efficiency of your cells’ powerhouses, leading to reduced energy levels and increased vulnerability to age-related issues.
What Is Mitochondrial Dysfunction?
Mitochondrial dysfunction occurs when these organelles fail to produce adequate energy. Key metrics like ATP output, membrane potential, and ROS balance are disrupted. For example, studies show that muscle mitochondrial density decreases by 15% in older adults compared to younger individuals.
How Aging Leads to Mitochondrial Decline
As you age, the efficiency of the electron transport chain declines. Complexes I and III, crucial for energy production, become less effective. This decline is exacerbated by the accumulation of reactive oxygen species (ROS), which damage mitochondrial DNA and proteins. This creates a vicious cycle, further impairing function.
The Impact of Reactive Oxygen Species (ROS)
ROS are byproducts of energy production that can cause oxidative damage if not properly managed. In aging cells, ROS levels often exceed the body’s ability to neutralize them. This imbalance damages the electron transport chain and accelerates mitochondrial decline. Research on SOD2-deficient mice, which lack a key antioxidant enzyme, shows a 30% reduction in lifespan due to increased ROS damage.
Additionally, studies like the CALERIE trial highlight the benefits of interventions like caloric restriction and exercise, which reduce cardiovascular risk by 38% and improve mitochondrial health. These findings underscore the importance of proactive measures to support cellular function as you age.
How Aging Affects Mitochondria and Fat Storage
As you grow older, your body’s ability to process and store fat undergoes significant changes. These shifts are closely tied to the health of your mitochondria, the energy powerhouses of your cells. Over time, mitochondrial dysfunction can disrupt fat metabolism, leading to changes in how your body manages energy and weight.
The Connection Between Mitochondria and Fat Metabolism
Mitochondria play a key role in breaking down fats through a process called β-oxidation. In younger individuals, this process is efficient, converting fats into energy effectively. However, as you age, the efficiency of β-oxidation declines. Studies show that aged adipocytes (fat cells) struggle to process fats, leading to fat storage rather than energy production.
How Fat Storage Changes with Age
Fat storage patterns shift dramatically over time. In your 20s, fat is primarily stored under the skin (subcutaneous fat). By your 70s, visceral fat—fat around your organs—increases by 200%. This type of fat is linked to higher risks of obesity and metabolic disorders. Additionally, ectopic fat deposition in muscles and the liver becomes more common, further complicating metabolism.
The Role of Mitochondria in Age-Related Weight Gain
Mitochondrial health directly impacts weight management. As mitochondria become less efficient, they produce more reactive oxygen species (ROS). This oxidative stress can lead to insulin resistance, making it harder for your body to regulate blood sugar and fat storage. Research also shows a 22% lower M-value in older adults during hyperinsulinemic clamps, indicating reduced insulin sensitivity.
Understanding these changes can help you take proactive steps to support your metabolism and maintain a healthy weight as you age.
Mitochondrial DNA Mutations and Aging
Mitochondrial DNA plays a crucial role in your cellular energy production, but it’s not immune to damage. Over time, mutations in this DNA can lead to significant declines in mitochondrial function. Understanding these changes is key to addressing age-related health issues.
What Are Mitochondrial DNA Mutations?
Mitochondrial DNA (mtDNA) contains 37 genes responsible for energy production. Unlike nuclear DNA, mtDNA lacks histone protection, making it more susceptible to damage. Mutations in these genes can disrupt the electron transport chain, reducing ATP production.
For example, POLG mutator mice, which have defective mtDNA repair mechanisms, show a 50% reduction in lifespan. This highlights the critical role of mtDNA integrity in cellular health.
How Mutations Accumulate Over Time
Mutations in mtDNA accumulate through a process called replicative segregation. When mitochondria divide, mutated and healthy mtDNA are randomly distributed. Over time, cells with a high percentage of mutated mtDNA become dysfunctional.
Studies show that aged human neurons have 1.5 times more mtDNA deletions than younger cells. This accumulation often exceeds the 60% threshold required to impair mitochondrial function significantly.
The Impact of Mutations on Mitochondrial Function
When mutations exceed the threshold, they disrupt energy production and increase oxidative damage. This can lead to diseases like atherosclerosis, where leukocyte heteroplasmy (mixed mtDNA populations) is a contributing factor.
Research contrasts linear and exponential models of mutation accumulation. While linear models suggest gradual damage, exponential models indicate rapid deterioration in later years.
| Key Concept | Description |
|---|---|
| mtDNA Structure | 37 genes, no histone protection. |
| Replicative Segregation | Random distribution of mutated and healthy mtDNA. |
| Threshold Effect | Over 60% mutated mtDNA impairs function. |
| Mutation Models | Linear vs. exponential accumulation. |
“Mitochondrial DNA mutations are a silent driver of cellular aging, often overlooked until dysfunction becomes apparent.”
By understanding these mechanisms, you can take steps to protect your mitochondrial DNA and maintain cellular health as you age.
Reactive Oxygen Species (ROS) and Oxidative Stress
Reactive oxygen species (ROS) are natural byproducts of cellular energy production, but their balance is crucial for health. When produced in moderation, ROS act as signaling molecules, supporting cellular functions. However, excessive ROS can lead to oxidative stress, damaging cells and accelerating aging.

What Are Reactive Oxygen Species?
ROS include molecules like superoxide, hydrogen peroxide (H2O2), and hydroxyl radicals. These molecules are generated during energy production in the mitochondrial membrane. While they play roles in immune defense and cell signaling, their overproduction can harm lipids, proteins, and DNA.
For example, the Fenton reaction converts H2O2 into highly reactive hydroxyl radicals, which can damage phospholipid membranes. This process is a key driver of cellular damage.
How ROS Contributes to Aging
As you age, your body’s ability to neutralize ROS declines. This imbalance leads to oxidative stress, which damages mitochondrial DNA and proteins. Studies show that Mn-SOD overexpression extends mouse lifespan by 20%, highlighting the importance of ROS regulation.
Additionally, HIF-1 activation in C. elegans increases longevity by 40%, demonstrating the role of ROS in aging pathways. However, when ROS levels exceed the body’s antioxidant capacity, they accelerate cellular aging.
The Role of Antioxidants in Mitigating ROS
Antioxidants like astaxanthin and CoQ10 help neutralize ROS, reducing oxidative stress. Research shows that NRF2 activation through caloric restriction enhances antioxidant defenses, protecting cells from damage.
Human trials also support the efficacy of antioxidants in improving mitochondrial health. For instance, CoQ10 supplementation has been shown to reduce ROS levels and improve energy production in older adults.
| ROS Type | Effect |
|---|---|
| Superoxide | Initiates oxidative chain reactions. |
| Hydrogen Peroxide (H2O2) | Converted to hydroxyl radicals via Fenton reaction. |
| Hydroxyl Radicals | Highly reactive, damages lipids, proteins, and DNA. |
“The balance between ROS production and antioxidant defenses is critical for maintaining cellular health and longevity.”
Understanding the role of ROS and oxidative stress can help you take steps to support your cellular health as you age.
Mitochondrial Biogenesis and Aging
Mitochondrial biogenesis is your body’s way of renewing its energy factories. This process involves creating new mitochondria to replace damaged or inefficient ones. As you age, this renewal process slows, leading to reduced energy production and cellular health.
What Is Mitochondrial Biogenesis?
Mitochondrial biogenesis is regulated by a signaling cascade involving PGC-1α, NRF1, and TFAM. These proteins work together to activate genes responsible for mitochondrial growth and function. For example, PGC-1α stimulates the production of proteins essential for energy production.
Studies show that trained elderly individuals have 38% higher levels of OXPHOS proteins compared to sedentary peers. This highlights the importance of maintaining mitochondrial biogenesis for energy efficiency.
How Biogenesis Declines with Age
As you age, the efficiency of mitochondrial biogenesis decreases. Factors like reduced PGC-1α activity and lower TFAM expression contribute to this decline. Caloric restriction has been shown to increase TFAM expression by 2.1x in human trials, offering a potential solution.
Additionally, SIRT1, a protein involved in cellular health, plays a role in activating biogenesis through deacetylation. However, its activity diminishes with age, further impairing the process.
Strategies to Enhance Mitochondrial Biogenesis
Several strategies can help boost mitochondrial biogenesis:
- Exercise: High-intensity interval training (HIIT) and endurance training are particularly effective. HIIT has been shown to increase biogenesis by 27% in some studies.
- Caloric restriction: Reducing calorie intake without malnutrition enhances biogenesis by activating SIRT1 and increasing TFAM expression.
- Cold exposure: Brief exposure to cold temperatures can stimulate biogenesis by up to 27%.
- Supplements: Nicotinamide riboside, a precursor to NAD+, supports mitochondrial health and biogenesis.
By incorporating these strategies, you can support your cellular energy production and maintain vitality as you age.
Mitochondrial Dynamics: Fission and Fusion
Your cells rely on a delicate balance of processes to maintain energy and health, and mitochondrial dynamics play a central role. These dynamics involve two key processes: fission and fusion. Together, they ensure your mitochondria remain functional and efficient, even as you age.
Understanding Mitochondrial Fission and Fusion
Fission is the process by which mitochondria divide, while fusion allows them to merge. These processes are regulated by specific proteins. For example, Drp1 drives fission, while OPA1 and Mfn1-2 facilitate fusion. Together, they maintain mitochondrial quality and function.
Fission helps remove damaged parts of mitochondria, while fusion allows healthy components to combine, creating more efficient organelles. This balance is crucial for cellular health.
How Aging Disrupts Mitochondrial Dynamics
As you age, the balance between fission and fusion is disrupted. For instance, Mfn2 expression declines by 40% in Alzheimer’s patients, impairing fusion. This leads to fragmented mitochondria, reducing their efficiency.
Additionally, changes in Drp1 phosphorylation can alter fission rates. This imbalance contributes to oxidative stress and cellular damage, accelerating aging.
The Role of Mitophagy in Cellular Health
Mitophagy is the process of removing damaged mitochondria through autophagy. It relies on markers like p62 and LC3-II to identify and degrade dysfunctional organelles. For example, Parkin recruitment, which requires a 60mV membrane potential loss, is a key step in this process.
Compounds like urolithin A can enhance mitophagy by up to 30%, supporting cellular health. This process is essential for maintaining energy production and reducing damage.
| Protein | Role |
|---|---|
| Drp1 | Drives mitochondrial fission. |
| OPA1/Mfn1-2 | Facilitates mitochondrial fusion. |
| Parkin | Recruits autophagosomes for mitophagy. |
“Mitochondrial dynamics are the cornerstone of cellular health, ensuring damaged organelles are replaced and energy production remains efficient.”
By understanding these processes, you can take steps to support your mitochondrial health and maintain vitality as you age.
Mitochondria and Skeletal Muscle Aging
Your skeletal muscle health is deeply connected to the efficiency of your cellular powerhouses. As you age, the ability of these muscles to function optimally declines, largely due to changes in mitochondrial function. Understanding this relationship can help you take steps to maintain muscle strength and vitality.
How Aging Impacts Muscle Mitochondria
With age, the density of mitochondria in skeletal muscle decreases, particularly in type II fibers. Studies show a 22% reduction in mitochondrial density in these fibers. This decline is linked to reduced energy production and increased fatigue.
Additionally, the myonuclear domain theory explains how muscle atrophy occurs. As muscle fibers shrink, the number of nuclei remains constant, leading to an imbalance that further impairs function. This process is exacerbated by apoptosis, where damaged cells self-destruct.
The Role of Mitochondria in Muscle Atrophy
Muscle atrophy is a common issue as you grow older. One key factor is the activation of caspase-3, a protein involved in cell death. This activation is often triggered by disuse or inactivity, leading to muscle loss.
Research also highlights the role of the MOTS-c peptide in maintaining muscle homeostasis. This peptide supports mitochondrial health, helping to counteract the effects of aging on skeletal muscle.
Exercise and Mitochondrial Health in Aging
Regular exercise is one of the most effective ways to support mitochondrial health. Studies show that 12 weeks of resistance training can reverse 15% of mitochondrial loss in older adults. This improvement is linked to enhanced energy production and muscle strength.
Comparisons between neuromuscular electrical stimulation (NMES) and voluntary contractions reveal that both methods can boost mitochondrial function. However, voluntary contractions tend to be more effective in promoting long-term muscle health.
“Exercise not only preserves muscle mass but also enhances mitochondrial efficiency, offering a powerful tool against aging.”
By incorporating regular physical activity into your routine, you can support your skeletal muscle and maintain vitality as you age.
Mitochondria and Fat Storage: The Metabolic Link
Your body’s ability to manage energy and fat storage is deeply tied to mitochondrial health. These cellular powerhouses play a central role in breaking down fats and converting them into usable energy. Over time, changes in mitochondrial function can significantly alter how your body processes and stores fat.
How Mitochondria Regulate Fat Metabolism
Mitochondria break down fats through a process called β-oxidation. This process is essential for converting fatty acids into energy. In younger individuals, β-oxidation is highly efficient, but as you age, this efficiency declines. Studies show that fat oxidation rates can drop by 50% in older adults compared to younger individuals.
One key regulator of fat metabolism is CPT1, a protein that transports fatty acids into mitochondria. When CPT1 activity decreases, fats are less likely to be used for energy and more likely to be stored. Additionally, UCP1, a protein in brown adipose tissue, helps generate heat by burning fat. However, its activity decreases with age, further reducing fat metabolism.
The Impact of Aging on Fat Storage
As you grow older, your body’s fat storage patterns shift. Subcutaneous fat, stored under the skin, decreases, while visceral fat, around your organs, increases. This type of fat is linked to higher risks of obesity and metabolic disorders.
Ectopic fat deposition, where fat accumulates in muscles and the liver, also becomes more common. This can lead to insulin resistance, making it harder for your body to regulate blood sugar. Research shows that obese individuals have 3x higher ceramide levels in their adipose tissue, which further impairs metabolism.
Mitochondrial Dysfunction and Obesity
When mitochondria become less efficient, they produce more reactive oxygen species (ROS). This oxidative stress can damage cellular components and contribute to obesity. For example, ROS can activate PKCθ, a protein that disrupts insulin signaling and promotes fat storage.
Additionally, FGF21 resistance in metabolic syndrome reduces the body’s ability to burn fat. Time-restricted feeding trials have shown promise in improving mitochondrial function and reducing fat storage. These findings highlight the importance of maintaining mitochondrial health for weight management.
| Key Factor | Impact on Fat Storage |
|---|---|
| CPT1 Activity | Regulates fatty acid transport into mitochondria. |
| UCP1 Downregulation | Reduces fat burning in brown adipose tissue. |
| Ectopic Fat Deposition | Increases insulin resistance and metabolic risks. |
| ROS Production | Promotes oxidative stress and fat storage. |
“Mitochondrial health is the cornerstone of efficient fat metabolism and energy regulation.”
By understanding these processes, you can take steps to support your mitochondrial function and maintain a healthy weight as you age.
Insulin Sensitivity and Mitochondrial Health
Insulin sensitivity plays a pivotal role in your body’s ability to manage energy and health. When your cells respond effectively to insulin, they can efficiently absorb glucose, maintaining stable blood sugar levels. However, this process relies heavily on the health of your mitochondria, the energy powerhouses of your cells.
As you age, the connection between insulin signaling and mitochondrial function becomes increasingly important. Changes in mitochondrial efficiency can directly impact how your body processes glucose, leading to metabolic imbalances. Understanding this relationship is key to maintaining your health over time.
The Role of Mitochondria in Insulin Signaling
Mitochondria are essential for the IRS1/PI3K/Akt pathway, which regulates insulin signaling. When insulin binds to its receptor, this pathway activates, allowing glucose to enter cells. Healthy mitochondria support this process by providing the energy needed for these cellular activities.
However, mitochondrial dysfunction can disrupt this pathway. For example, reduced ATP production impairs the ability of cells to respond to insulin. This can lead to insulin resistance, a precursor to type 2 diabetes.
How Aging Affects Insulin Sensitivity
As you grow older, your body’s ability to respond to insulin naturally declines. Studies show that elderly individuals have 22% lower M-values during hyperinsulinemic clamp studies, indicating reduced insulin sensitivity. This decline is often linked to changes in mitochondrial function.
One contributing factor is the accumulation of diacylglycerol in cells, which interferes with insulin signaling. Additionally, oxidative stress from ROS can damage mitochondrial DNA, further impairing their ability to support glucose uptake.
Mitochondrial Dysfunction and Type 2 Diabetes
Type 2 diabetes is closely tied to mitochondrial dysfunction. Patients with this condition often show a 40% reduction in OXPHOS capacity, the process by which mitochondria produce energy. This decline exacerbates insulin resistance, creating a vicious cycle.
Interventions like metformin and exercise can improve mitochondrial health by activating AMPK, a protein that enhances energy production. For example, trials with mitoQ, a mitochondrial antioxidant, have shown an 18% reduction in HbA1c levels, a key marker of diabetes control.
| Key Factor | Impact on Insulin Sensitivity |
|---|---|
| IRS1/PI3K/Akt Pathway | Regulates glucose uptake into cells. |
| Diacylglycerol Accumulation | Interferes with insulin signaling. |
| ROS Production | Damages mitochondrial DNA, impairing function. |
“Mitochondrial health is the cornerstone of efficient insulin signaling and glucose metabolism.”
By understanding these mechanisms, you can take steps to support your mitochondrial function and maintain healthy insulin sensitivity as you age.
Caloric Restriction and Mitochondrial Longevity
Caloric restriction has emerged as a powerful tool for enhancing cellular health and longevity. By reducing calorie intake by 20-40%, you can activate pathways that support cellular renewal and energy efficiency. This practice goes beyond weight management, offering a unique approach to improving mitochondrial function and overall vitality.

What Is Caloric Restriction?
Caloric restriction involves reducing daily calorie intake without compromising essential nutrients. Typically, this means consuming 20-40% fewer calories than your body requires for maintenance. This approach has been shown to activate sirtuins, proteins that play a key role in cellular health and longevity.
For example, the CALERIE trial demonstrated a 27% reduction in mtDNA damage among participants practicing caloric restriction. This highlights its potential to mitigate oxidative damage and support mitochondrial health.
How Caloric Restriction Affects Mitochondria
Caloric restriction enhances mitochondrial function by increasing SIRT1 activity. In human monocytes, SIRT1 levels rise by 3.2x during caloric restriction, promoting cellular repair and energy efficiency. Additionally, this practice inhibits mTOR, a protein that regulates cell growth and proteostasis, further supporting mitochondrial health.
Circadian alignment also plays a synergistic role. By aligning calorie intake with your body’s natural rhythms, you can optimize mitochondrial biogenesis and energy production. This approach has been shown to enhance mitophagy markers, as seen in fasting-mimicking diet (FMD) trials.
The Role of Caloric Restriction in Aging
Caloric restriction slows aging by reducing oxidative damage and enhancing cellular repair mechanisms. It also promotes longevity by activating pathways that support mitochondrial biogenesis and energy efficiency. For instance, protein restriction, a subset of caloric restriction, has been shown to extend lifespan in animal models.
Comparisons between global caloric restriction and protein restriction reveal unique benefits. While both approaches improve mitochondrial function, global caloric restriction offers broader metabolic advantages. FMD trials further support this, showing significant improvements in mitophagy markers and cellular health.
| Key Benefit | Impact |
|---|---|
| SIRT1 Activation | Enhances cellular repair and energy efficiency. |
| mTOR Inhibition | Supports proteostasis and mitochondrial health. |
| Circadian Alignment | Optimizes mitochondrial biogenesis and energy production. |
| Mitophagy Markers | Improves cellular renewal and reduces oxidative damage. |
“Caloric restriction is not just about eating less—it’s about activating pathways that support cellular vitality and longevity.”
By incorporating caloric restriction into your lifestyle, you can support your mitochondrial health and maintain vitality as you age.
Exercise: A Key to Mitochondrial Health
Exercise isn’t just about staying fit—it’s a powerful tool for enhancing cellular energy production. Regular physical activity supports your mitochondrial function, helping your body generate and use energy more efficiently. This is especially important as you age, when cellular energy production naturally declines.

How Physical Activity Boosts Mitochondrial Function
When you engage in exercise, your body activates pathways like AMPK-PGC1α-FNDC5/irisin. These pathways stimulate mitochondrial biogenesis, the process of creating new mitochondria. For example, high-intensity interval training (HIIT) increases PGC-1α levels by 2.5x compared to steady-state cardio.
Lactate, often seen as a byproduct of intense exercise, also plays a role. It acts as a fuel source for mitochondria, supporting energy production during and after workouts. This process helps improve recovery and overall cellular efficiency.
The Role of Exercise in Fat Metabolism
Physical activity enhances fat metabolism by improving the efficiency of β-oxidation, the process by which fats are broken down for energy. Zone 2 training, which focuses on moderate intensity, is particularly effective for boosting fat utilization.
In contrast, VO2 max training, which pushes your aerobic capacity, improves overall cardiovascular health. Both methods support mitochondrial health, but they target different aspects of energy production and fat metabolism.
Exercise and Aging: What You Need to Know
As you age, maintaining an active lifestyle becomes even more critical. Studies show that a 6-month cycling protocol can reverse 17% of phosphocreatine (PCr) recovery, a marker of mitochondrial efficiency. This highlights the restorative power of regular exercise.
Cold-water immersion is another strategy that can enhance recovery and mitochondrial function. It reduces inflammation and supports cellular repair, making it a valuable addition to your fitness routine.
| Training Type | Benefits |
|---|---|
| HIIT | Boosts PGC-1α levels, enhancing mitochondrial biogenesis. |
| Zone 2 Training | Improves fat metabolism and energy efficiency. |
| VO2 Max Training | Enhances cardiovascular health and aerobic capacity. |
| Cold-Water Immersion | Supports recovery and reduces inflammation. |
“Exercise is not just a way to stay fit—it’s a pathway to maintaining cellular vitality and energy efficiency as you age.”
By incorporating these strategies into your routine, you can support your skeletal muscle health, reduce ROS damage, and maintain vitality as you grow older.
Mitochondrial Therapies and Aging
Advancements in science are unlocking new ways to support your cellular energy systems. From cutting-edge therapies to targeted supplements, researchers are exploring innovative solutions to enhance mitochondrial health and combat age-related decline.
Emerging Therapies for Mitochondrial Health
One promising approach is the use of peptides like SS-31, which improves electron transport chain efficiency by 40%. Another breakthrough is MitoQ, a mitochondrial-targeted antioxidant that reduces 6MWT decline by 22% in elderly individuals. These therapies aim to restore cellular energy production and reduce oxidative damage.
Gene therapy is also gaining traction, particularly for addressing mitochondrial dna mutations. By repairing or replacing damaged genes, this method could potentially reverse mitochondrial dysfunction and improve overall health.
The Role of Supplements in Mitochondrial Function
Supplements like NAD+ precursors and antioxidants are becoming popular for their ability to support mitochondrial health. For example, Urolithin A, currently in phase III trials, has shown promise in enhancing mitophagy, the process of removing damaged mitochondria.
Other compounds, such as CoQ10 and astaxanthin, help neutralize reactive oxygen species, reducing oxidative stress. These supplements offer a practical way to support cellular energy production and longevity.
Future Directions in Mitochondrial Research
The future of mitochondrial research is focused on understanding the mechanisms of aging and developing targeted interventions. Scientists are exploring the pharmacokinetics of NAD+ precursors and comparing dietary approaches like dichloroacetate and ketogenic diets.
Additionally, research into mitophagy-inducing phytochemicals could lead to new therapies for age-related diseases. By combining these findings with lifestyle changes, we can unlock new ways to maintain vitality as we age.
“The future of mitochondrial health lies in the synergy of cutting-edge therapies, targeted supplements, and groundbreaking research.”
Lifestyle Changes to Support Mitochondrial Health
Your daily habits have a direct impact on your cellular energy systems. By making thoughtful adjustments to your routine, you can enhance the efficiency of your mitochondria and maintain vitality as you age. Let’s explore how diet, sleep, and stress management can support your cellular health.
Diet and Mitochondrial Function
What you eat plays a crucial role in supporting your mitochondria. The Mediterranean diet, rich in polyphenols and healthy fats, has been shown to increase electron transport chain complexes by 33%. Incorporating foods like olive oil, nuts, and leafy greens can provide essential nutrients that boost energy production.
Timing your meals also matters. Consuming polyphenol-rich foods earlier in the day can optimize their benefits. Additionally, including lean proteins and antioxidants in your meals helps repair cellular damage and supports mitochondrial efficiency.
The Role of Sleep in Mitochondrial Health
Quality sleep is essential for cellular repair and energy balance. Studies show that just 5 hours of sleep can reduce Complex IV activity by 19%, impairing mitochondrial function. Prioritizing 7-9 hours of restful sleep allows your body to perform essential maintenance tasks, such as mitophagy, the process of removing damaged mitochondria.
Melatonin, a hormone produced during sleep, plays a key role in this process. To support your circadian rhythm, consider reducing blue light exposure before bed and creating a consistent sleep schedule.
Stress Management and Mitochondrial Longevity
Chronic stress can take a toll on your cellular health by increasing oxidative damage. The HPA axis, which regulates stress responses, interacts with mitochondrial function. Managing stress through practices like meditation, yoga, or even sauna sessions can help. Saunas, for example, induce heat shock proteins like HSP70, which support cellular repair.
By balancing your stress levels, you can reduce the production of reactive oxygen species and promote mitochondrial longevity. Simple strategies like deep breathing or spending time in nature can make a significant difference.
“Your lifestyle choices today shape the health of your mitochondria tomorrow. Small changes can lead to lasting benefits.”
Conclusion: Taking Control of Your Mitochondrial Health
Taking proactive steps to support your cellular energy systems can significantly enhance your overall well-being. Managing reactive oxygen species (ROS) is crucial, as it reduces oxidative damage and supports mitochondrial health. Aim for at least 150 minutes of exercise weekly to boost energy production and maintain vitality.
Regular testing, such as quarterly DEXA scans, can help monitor your cellular health. Advances like CRISPR-based mtDNA editing offer promising strategies for addressing genetic mutations and improving function. Pair these innovations with a balanced diet rich in antioxidants and lean proteins for optimal results.
Here’s a simple 5-point plan: exercise regularly, eat nutrient-dense foods, manage stress, prioritize sleep, and stay informed about new therapies. By adopting these habits, you can take control of your mitochondrial health and thrive as you age.