Did you know 25% of men and 10% of women aged 30-70 in the U.S. struggle with disrupted breathing at night? Many dismiss loud nighttime sounds as harmless, but they could signal a serious condition. Left unchecked, this issue raises risks for heart disease and stroke by up to 60%.
Partners often notice symptoms first—gasps for air or abrupt silences during rest. Morning headaches affect 30% of patients, caused by low oxygen levels. The Cleveland Clinic reports 80% of moderate-to-severe cases go undiagnosed, delaying life-changing treatment.
Recognizing early signs can slash daytime fatigue by 70% and lower accident risks. This guide explores key indicators, diagnostic steps, and modern solutions to restore healthy rest.
Key Takeaways
- Millions experience undiagnosed breathing disruptions during rest.
- Untreated conditions heighten cardiovascular dangers significantly.
- Loved ones frequently observe warning signals before patients do.
- Morning headaches may indicate overnight oxygen deprivation.
- Proper care dramatically improves energy and safety.
Understanding Snoring and Sleep Apnea
Throat muscle relaxation during rest can trigger dangerous airflow blockages. Snoring occurs when tissues partially obstruct the airway, while obstructive sleep apnea (OSA) involves complete pauses in breathing for 10+ seconds.
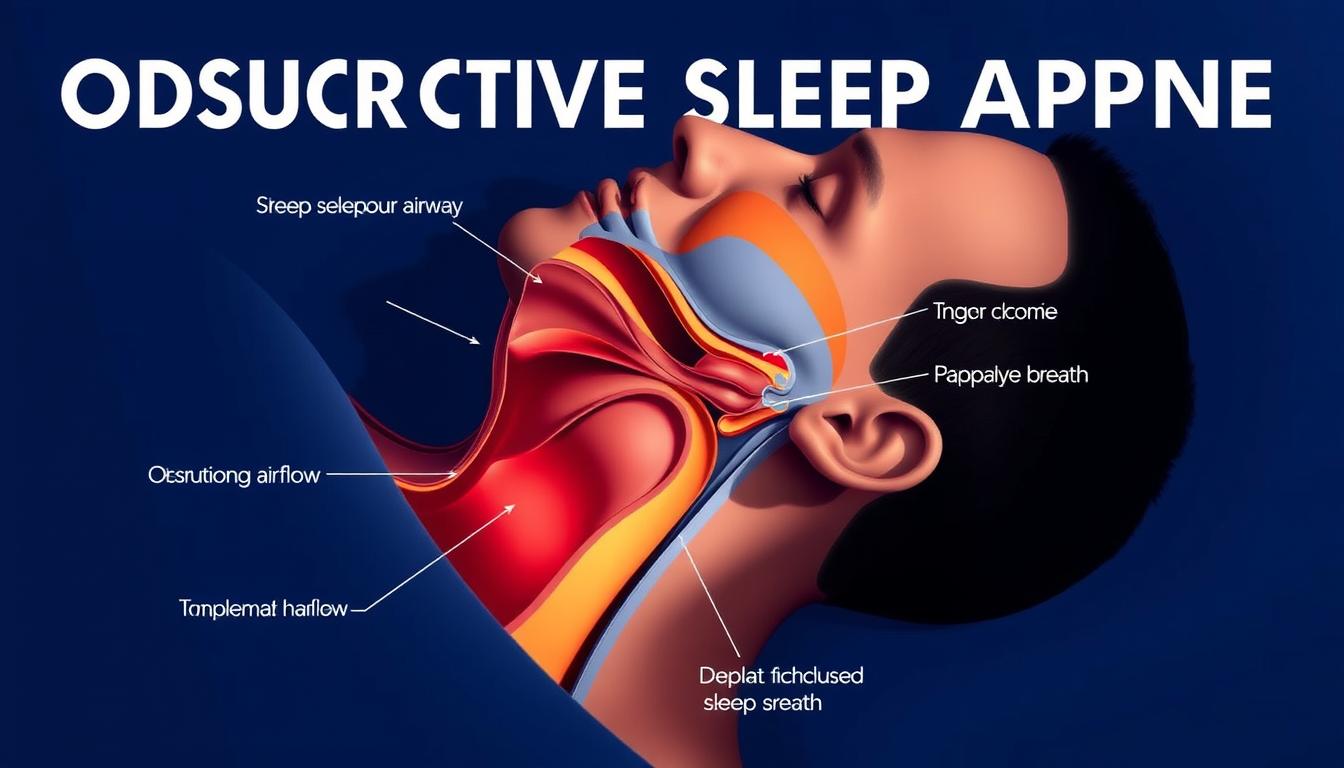
During OSA, the windpipe collapses, cutting off oxygen. The brain jolts you awake to restart breathing—sometimes 100+ times nightly. Cleveland Clinic notes oxygen levels may plummet below 80%, straining the heart and brain.
How Apneic Events Disrupt Sleep
| Event Type | Duration | Frequency/Hour | Oxygen Drop |
|---|---|---|---|
| Normal Breathing | Steady | 0–5 | >95% |
| Mild OSA | 10–20 sec | 5–15 | 85–90% |
| Severe OSA | 30+ sec | 30+ |
REM sleep worsens obstructive sleep apnea because muscles relax further. Geisinger researchers found 70% of OSA patients also battle obesity, which narrows the airway.
Untreated apnea costs $3.4 billion yearly in U.S. healthcare. Unlike OSA, central apnea stems from faulty brain signals—not physical blockages.
Key Warning Signs of Sleep Apnea
Your body sends distress signals when breathing stops during rest. These symptoms often go unnoticed but can escalate health risks. Recognizing them early helps you seek timely care.

Loud or Chronic Snoring
Snoring exceeding 40 decibels—like a refrigerator hum—affects 90% of patients. A partner may notice it first. Persistent sounds suggest throat tissues obstruct airflow.
Gasping or Choking During Sleep
When oxygen levels crash, your brain jolts you awake to restart breathing. These gasps reflect emergency responses to airway blockages.
Excessive Daytime Fatigue
Even 8 hours in bed may leave you exhausted. Microarousals disrupt deep sleep cycles. 68% of patients report unrefreshing rest, raising accident risks 2.5-fold.
Morning Headaches or Dry Mouth
CO2 buildup dilates blood vessels, triggering headaches. Dry mouth stems from mouth breathing when nasal passages fail.
Frequent Nighttime Urination
Hormonal surges during apnea episodes cause nocturia. 50% of patients wake repeatedly to urinate, fracturing sleep further.
“Epworth Sleepiness Scale scores above 10 warrant clinical evaluation.”
Risk Factors for Developing Sleep Apnea
Certain traits make you more likely to develop breathing disruptions at night. These risk factors range from biological traits to daily habits. Identifying them helps you take preventive steps.
Age, Gender, and Body Weight
Men face 2–3 times higher odds until menopause, per Cleveland Clinic. Neck size matters too—over 17 inches (men) or 16 inches (women) raises risks. Each 10% weight gain increases breathing pauses by 32% (Geisinger).
Lifestyle and Health Conditions
Alcohol relaxes throat muscles, worsening airway collapse. Half of patients have high blood pressure; 30% have diabetes. GERD often triggers and results from breathing disturbances.
- Racial disparities: Higher prevalence in Black communities.
- Postmenopausal women: Risk matches men due to hormonal shifts.
Genetics and Anatomy
Family history quadruples your odds. Physical traits like a recessed jaw or enlarged tonsils narrow the airway. 40% of cases tie to genetic factors (Cleveland Clinic).
“Neck circumference predicts apnea severity better than BMI in some populations.” — Geisinger Health System
Types of Sleep Apnea: Obstructive vs. Central
Not all nighttime breathing issues stem from the same root problem. Obstructive sleep apnea (OSA) involves physical blockages, while central sleep apnea (CSA) occurs when the brain fails to signal breathing muscles. Cleveland Clinic reports OSA accounts for 84% of diagnosed cases.

OSA happens when throat muscles relax, collapsing the airway. CSA often links to heart failure or opioid use. Geisinger notes opioid-induced CSA differs from Cheyne-Stokes respiration, a pattern tied to heart disease.
| Type | Cause | Prevalence | Key Trait |
|---|---|---|---|
| Obstructive (OSA) | Airway blockage | 25% men | Loud snoring |
| Central (CSA) | Brain signal failure | 0.9% general | Erratic breathing |
Complex sleep apnea combines both types. About 15% of CPAP users develop treatment-emergent central apneas. Unlike OSA, CSA patients rarely snore but show abrupt air flow changes.
Untreated CSA carries higher mortality risks than OSA. Inspire® implants target OSA, while Remedē® devices address CSA. Learn more about obstructive sleep solutions.
“Mixed apnea events require dual treatment approaches—addressing both mechanical and neurological triggers.” — Cleveland Clinic
How Sleep Apnea Is Diagnosed
Medical professionals use advanced tools to confirm nighttime breathing disorders. Accurate diagnosis helps determine treatment plans tailored to your needs. Testing evaluates breathing sleep patterns, oxygen levels, and event frequency.
Sleep Studies (Polysomnography)
In-lab sleep study tests monitor 16+ body functions. Sensors track brain waves, muscle activity, and airflow. The Cleveland Clinic notes these Type I studies are the gold standard.
| Study Type | Channels | Setting | Best For |
|---|---|---|---|
| Type I | 16+ | Lab | Complex cases |
| Type II | 7-15 | Home | Moderate severity |
| Type III | 4-7 | Home | Screening |
Home Sleep Apnea Tests
Portable devices detect 80-90% of moderate cases. Geisinger research shows they miss 35% of mild disorders. These Type III tests measure:
- Nasal airflow
- Chest movement
- Blood oxygen
“62% of home tests require follow-up lab studies for confirmation.”
When to Consult a Healthcare Provider
Seek a specialist if you experience:
- Observed breathing pauses
- Daytime fatigue with symptoms
- Refractory high blood pressure
Most insurers cover testing when Epworth scores exceed 8. Costs range from $150 for home tests to $3,000 for full polysomnography. Board-certified provider interpretation ensures accurate results.
Effective Treatment Options for Sleep Apnea
Modern medicine offers multiple approaches to restore nighttime breathing. Your treatment plan depends on severity, anatomy, and lifestyle factors. Combining methods often yields the best results for sustained restful sleep.
Lifestyle Adjustments That Make a Difference
Weight loss significantly improves airway function—a 10% reduction cuts breathing pauses by 26%. Sleeping on your side prevents tongue collapse in 56% of mild cases. Avoiding alcohol and sedatives before bed reduces throat muscle relaxation.
Geisinger studies show lifestyle changes combined with myofunctional therapy boost treatment success by 40%. Simple steps like nasal strips or allergy management can enhance nasal airflow.
Breathing Devices: CPAP and Beyond
CPAP machines eliminate 90% of events at 12 cm H2O pressure. The Cleveland Clinic reports 80-95% effectiveness when used consistently. Modern models feature humidification and auto-adjusting pressure for comfort.
Mandibular advancement devices (MADs) require at least 6mm jaw protrusion to work. These oral appliances suit mild-to-moderate cases and travelers who can’t use CPAP. Dentist-fitted options outperform store-bought versions.
Surgical Solutions for Lasting Relief
Uvulopalatopharyngoplasty (UPPP) removes excess throat tissue with 50% success rates. Maxillomandibular advancement (surgery) repositions the jaw, achieving 85% effectiveness for anatomical causes. Inspire® implants demonstrate 79% success over five years.
“Outpatient procedures now address airway obstructions with minimal recovery time,” notes a Cleveland Clinic report. Tonsillectomies help pediatric cases, while septoplasty fixes deviated septums.
The Future of Apnea Management
Hypoglossal nerve stimulation activates tongue muscles during sleep—a 3-hour outpatient procedure. Daytime neuromuscular electrical training shows promise for mild cases. Zepbound® medication reduces events by 63% in obese patients.
Combination therapies are gaining traction, like CPAP with positional trainers. Research continues on smart pillows that detect and prevent obstruction automatically.
“Personalized treatment plans based on sleep study data yield 72% better adherence than one-size-fits-all approaches.”
Conclusion: Taking Control of Your Sleep Health
Proactive steps today prevent serious health complications tomorrow. Early treatment slashes risk by 75%, per Cleveland Clinic data. Download sleep diaries or locate accredited centers to start your journey.
Medicare covers 80% of CPAP costs for qualifying patients. Avoid unverified OTC fixes—only clinically tested solutions address root causes. Annual check-ups matter, as 30% need therapy tweaks.
Compliance boosts productivity by 45% in six months. Proper care adds seven healthy life-years. Complete the STOP-BANG quiz now to assess your condition.
Partner with a provider to reclaim restful sleep. Your health deserves expert attention. Act today—your future self will thank you.