Did you know 1 in 8 women will develop a thyroid condition in their lifetime? This small butterfly-shaped gland controls metabolism, energy levels, and even body temperature. When it malfunctions, your entire system feels the effects.
Thyroid issues range from easily managed hormone imbalances to rare autoimmune diseases. Many people don’t realize fatigue, weight changes, or mood swings could signal glandular problems. Early detection often prevents complications.
Women face higher risks—they’re 5-8 times more likely than men to develop these conditions. But here’s the good news: most thyroid diseases respond well to treatment. Medication adjustments and regular monitoring help millions live symptom-free.
Your thyroid’s hormones influence every cell. From heart rate to digestion, this powerhouse drives critical bodily functions. Understanding warning signs empowers you to seek care before minor issues escalate.
Key Takeaways
- Thyroid conditions affect women disproportionately compared to men
- Early symptom recognition leads to better treatment outcomes
- Hormone imbalances impact multiple bodily systems simultaneously
- Most gland-related diseases are manageable with medical supervision
- Routine blood tests often detect problems before symptoms worsen
Understanding Your Thyroid Gland
A butterfly-shaped organ orchestrates your energy use and more. Located at the base of your neck, this vital structure weighs less than an ounce but directs critical bodily functions. Its strategic position allows doctors to check for abnormalities through simple physical exams.
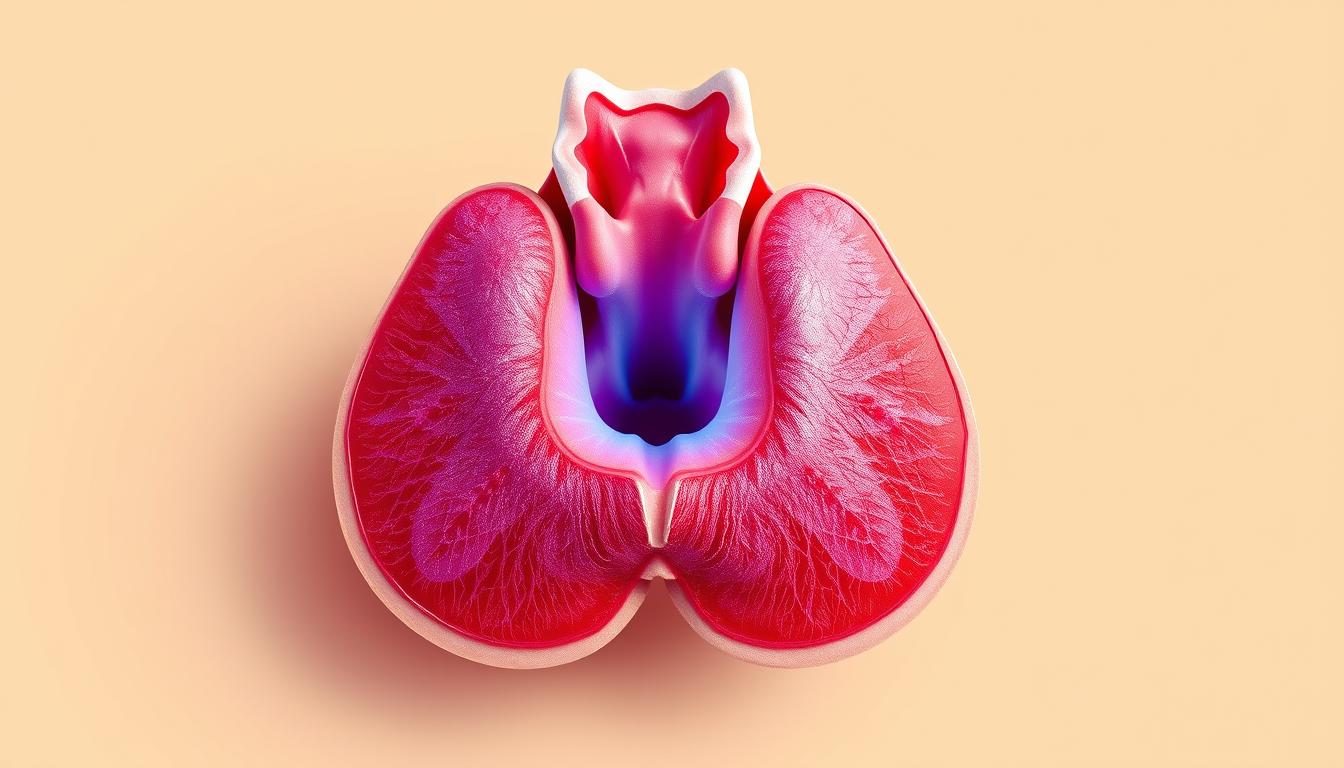
Anatomy and Function
Your gland measures about 2 inches wide, sitting below your Adam’s apple. It produces two key hormones: T3 (triiodothyronine) and T4 (thyroxine). These chemicals travel through your bloodstream, influencing cell activity everywhere from your brain to your toes.
| Hormone | Primary Function | Production Trigger |
|---|---|---|
| T3 | Directly powers cellular energy | TSH from pituitary gland |
| T4 | Converts to T3 as needed | Iodine intake + TSH signals |
Role in Metabolic Processes
This gland acts as your body’s thermostat and engine regulator. It determines how fast you burn calories, how warm you feel, and even how quickly your heart beats. Proper hormone balance ensures:
- Stable energy throughout the day
- Efficient nutrient processing
- Consistent organ performance
Your pituitary gland serves as the control center, adjusting TSH levels based on your body’s needs. When this system falters, every cell feels the impact – from sluggish digestion to irregular sleep patterns.
Common Thyroid Disorders Explained
Your body’s metabolic engine can malfunction in two primary ways. Hypothyroidism slows systems down like a car stuck in low gear, while hyperthyroidism revs functions into overdrive. These opposing conditions stem from hormone imbalances that affect nearly 1 in 10 Americans.
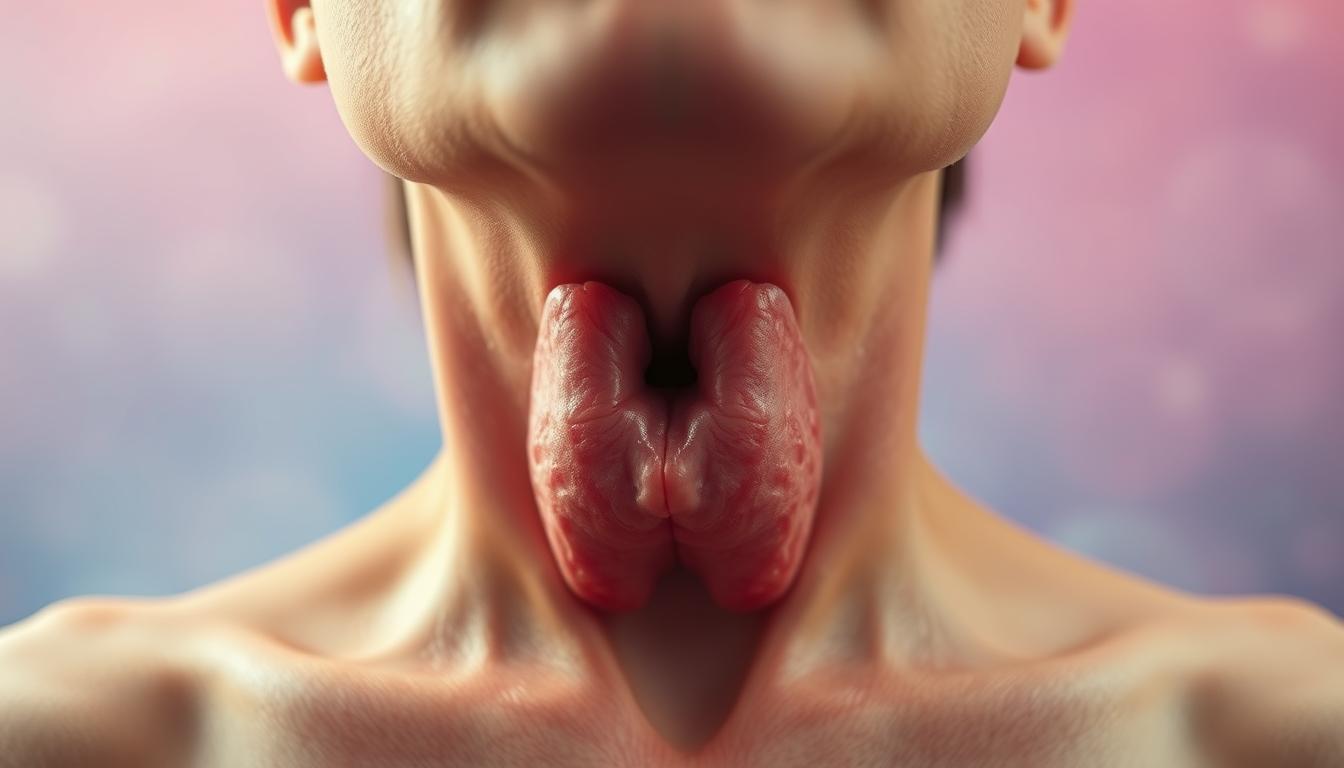
Definition and Scope of Thyroid Issues
Underactive gland function (hypothyroidism) impacts 5% of adults, often causing weight gain and fatigue. Overactivity (hyperthyroidism) affects fewer people but brings rapid heartbeat and anxiety. Both require blood tests for accurate diagnosis.
Structural changes complicate some cases. Enlarged glands (goiters) may develop visible neck swelling. Nodules form in 50% of individuals over 60, though most remain harmless. Thyroiditis inflammation sometimes triggers temporary hormone surges followed by crashes.
Women face 8x higher risk than men, particularly during hormonal shifts like pregnancy or menopause. Age increases vulnerability – most diagnoses occur after 40. Early treatment prevents heart complications and bone density loss.
Modern medicine offers effective solutions for these conditions. Synthetic hormones restore balance in underactive cases, while anti-thyroid medications calm excessive production. Regular monitoring helps maintain optimal levels long-term.
Identifying Thyroid Symptoms and Risk Factors
Your body sends signals when hormone balance shifts. Many miss early warnings because signs mirror everyday stress or aging. Knowing what patterns to watch helps catch issues before they escalate.
When Systems Accelerate
Hyperthyroidism makes your metabolism race like an unchecked engine. You might notice sudden weight loss despite normal eating. Heart palpitations often accompany shaky hands and excessive sweating.
Sleep troubles and frequent bathroom trips commonly occur. Some develop eye changes – lids may appear retracted or swollen. These symptoms typically develop gradually over weeks.
When Functions Slow Down
Hypothyroidism acts like a body-wide power saver mode. Unexplained weight gain and constant chilliness often appear first. Dry skin and thinning hair frequently accompany low energy levels.
Mental fog and forgetfulness can disrupt daily routines. Women might experience heavier periods or fertility challenges. Severe cases sometimes lead to visible neck swelling.
| Symptom Type | Hyperthyroidism | Hypothyroidism |
|---|---|---|
| Energy Level | Restlessness | Fatigue |
| Weight Changes | Loss | Gain |
| Temperature | Heat intolerance | Cold sensitivity |
| Heart Rate | Elevated | Slowed |
Certain factors raise your risk significantly. Women over 60 with autoimmune conditions need particular vigilance. Family history doubles your chances of developing gland issues.
If multiple symptoms persist for weeks, schedule blood tests. Early detection prevents complications like heart strain or osteoporosis. Proper management helps most people regain normal function.
Diagnosis and Testing for Thyroid Disorders
Modern medicine offers precise tools to uncover glandular imbalances. Accurate identification of issues begins with a combination of clinical evaluations and advanced technology. Three key approaches help medical professionals pinpoint problems effectively.
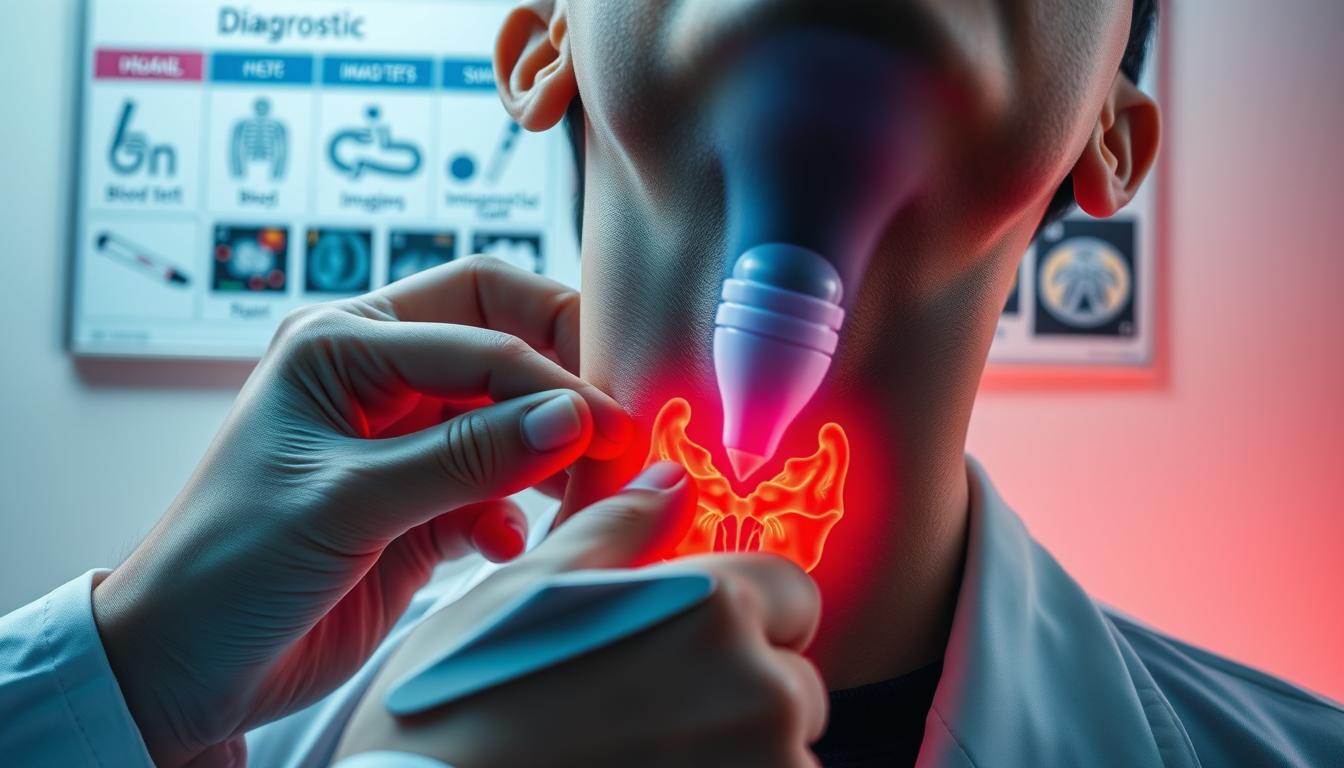
Blood Tests and Hormone Analysis
Thyroid-stimulating hormone (TSH) tests serve as the frontline diagnostic tool. Your doctor checks TSH levels alongside T3 and T4 hormones to assess gland performance. High TSH typically signals underactivity, while low TSH with elevated hormones suggests overproduction.
Specialized blood work detects antibodies linked to autoimmune conditions like Hashimoto’s. These tests often explain why hormone levels fluctuate despite normal gland structure.
Imaging and Physical Examinations
Your physician will gently palpate your neck during exams, feeling for unusual lumps or enlargement. Ultrasound imaging creates detailed pictures of gland structure, revealing nodules as small as 2 millimeters.
This painless procedure differentiates solid growths from fluid-filled cysts. Suspicious findings may lead to further testing, but most abnormalities prove harmless.
Iodine Uptake and Additional Diagnostic Methods
Radioactive iodine tests measure how efficiently your gland absorbs this crucial nutrient. Low uptake often confirms hypothyroidism, while excessive absorption indicates hyperactivity.
Advanced methods include:
- Fine-needle biopsies for questionable nodules
- Thyroid scans mapping hormone production areas
- 24-hour urine tests assessing iodine excretion
While self-checks using mirrors help spot visible swelling, always consult professionals for conclusive results. Early intervention prevents complications and restores balance.
Managing Thyroid Hormone Levels
Balancing your body’s chemical messengers requires precision and patience. Medical professionals use targeted approaches to restore equilibrium when production goes awry. Regular monitoring ensures your system stays finely tuned.
Medication and Radioactive Iodine Therapy
Radioactive iodine therapy offers a precise solution for overactive cells. You swallow a capsule that selectively targets problem areas without harming surrounding tissue. Most patients see hormone production normalize within 3-6 months.
| Treatment | How It Works | Time to Effect | Duration |
|---|---|---|---|
| Antithyroid Drugs | Blocks hormone production | 6-8 weeks | 12-18 months |
| Radioactive Iodine | Destroys overactive cells | 3-6 months | Single dose |
Antithyroid medications like methimazole provide faster symptom relief. “These drugs act like traffic controllers for hormone production,” explains Dr. Sarah Klein, an endocrinologist. Daily pills help 85% of patients achieve balance within a year.
Monitoring and Adjusting Hormone Levels
Your care team will schedule blood tests every 6-12 weeks initially. These checkups track three key markers:
- TSH (thyroid-stimulating hormone)
- Free T4 levels
- T3 concentrations when needed
Dosage adjustments become smaller as your numbers stabilize. Many people eventually need only annual checkups. Always take prescriptions at the same time daily—food interactions can reduce effectiveness by 40%.
“Successful management isn’t just about lab numbers—it’s how you feel day-to-day that truly matters.”
Keep a symptom journal to share with your doctor. Note energy patterns, temperature sensitivity, and sleep quality. This partnership helps fine-tune your treatment plan for optimal results.
Navigating Treatment Options: Hypothyroidism vs Hyperthyroidism
Treatment paths diverge significantly depending on whether your body produces too little or too much hormone. Managing these conditions requires tailored approaches that address root causes while minimizing side effects.
Thyroid Hormone Replacement Strategies
Hypothyroidism demands daily synthetic hormone pills like levothyroxine. This medication mimics natural T4, requiring precise dosing based on blood tests. Most patients start with low doses, increasing gradually over 6-8 weeks.
Key considerations for effective therapy:
- Take pills on an empty stomach for optimal absorption
- Avoid calcium supplements and antacids within 4 hours
- Report persistent fatigue or rapid heartbeat immediately
Dosage adjustments often occur during pregnancy or major weight changes. Annual checkups help maintain balance as you age.
Antithyroid Medications and Other Therapies
Hyperthyroidism treatments aim to slow hormone production or remove overactive tissue. Methimazole blocks hormone synthesis, while radioactive iodine selectively destroys malfunctioning cells.
| Treatment | Method | Long-Term Impact |
|---|---|---|
| Radioactive Iodine | Single capsule | Often leads to hypothyroidism |
| Thyroidectomy | Surgical removal | Requires lifelong hormone replacement |
Surgery becomes necessary when medications prove ineffective or for large goiters. Post-procedure, many patients transition to hormone pills. Those managing stress-related weight changes might explore certain supplements, though always consult your doctor first.
Understanding Thyroid Nodules and Goiters
Many adults discover unusual growths during routine neck exams without prior symptoms. These abnormalities often involve either small lumps or overall gland enlargement. While concerning at first glance, most prove manageable with proper medical guidance.
Causes and Characteristics of Thyroid Nodules
Nodules form as solid or fluid-filled lumps within your gland. Half of adults over 60 develop them, though fewer than 5% become cancerous. Radiation exposure and iodine deficiency remain leading contributors, particularly in regions with mineral-poor soil.
Genetic factors play roles in some cases. Autoimmune conditions like Hashimoto’s frequently trigger nodule formation. Though most cause no discomfort, larger growths may create visible swelling or swallowing difficulties.
Treatment Considerations for Goiters
Enlarged glands often signal underlying hormone imbalances. Your doctor might recommend watchful waiting for stable cases without symptoms. Medication adjustments frequently reduce swelling caused by hypoactive or hyperactive conditions.
Surgical removal becomes necessary when breathing or eating challenges develop. Modern techniques minimize scarring while addressing problematic tissue. Remember – most growths require monitoring rather than intervention.