One in eight women will develop thyroid issues during her lifetime, yet 60% of Americans with hormonal imbalances don’t realize they’re affected. This invisible epidemic often stems from unexpected sources – including the bread on your plate.
Autoimmune reactions drive most thyroid conditions, with research showing these processes account for over 80% of diagnosed cases. What many don’t realize? The proteins found in common foods can mimic thyroid tissue structure, confusing your body’s defenses.
Your metabolic command center works nonstop to regulate energy levels, weight, and even mood. When foreign particles enter your bloodstream through compromised digestion, they may spark cross-reactive immune attacks. This creates a chain reaction that disrupts hormone production.
Women face unique risks due to hormonal fluctuations throughout life stages. Awareness of dietary influences becomes critical when 5-8 times more likely to develop glandular dysfunction than men. Emerging studies reveal specific food components might accelerate this vulnerability.
Key Takeaways
- Autoimmune responses cause most thyroid disorders
- Millions remain undiagnosed despite clear symptoms
- Women’s biology increases susceptibility
- Digestive issues can trigger systemic inflammation
- Dietary choices may worsen hidden conditions
Introduction to Thyroid Health and Gluten
Nestled in your neck, a butterfly-shaped gland orchestrates energy use across every cell. This endocrine powerhouse produces T3 and T4 hormones that act like biological text messages – delivering instructions to your heart, brain, and digestive tract.
Hormonal Messengers at Work
Your gland releases these chemical signals constantly, maintaining core temperature and calorie burning rates. Even minor imbalances can trigger fatigue, weight fluctuations, or mood changes. Every organ system depends on precise hormonal communication to function optimally.

Ubiquitous Grain Proteins
Modern diets contain unprecedented amounts of wheat-derived substances. Gliadin and glutenin proteins form stretchy networks in baked goods, giving bread its chewy texture. These compounds now appear in sauces, processed meats, and even cosmetics.
While whole grains offer nutritional benefits, refined flour products dominate supermarket shelves. Many consume gluten daily without recognizing potential effects on delicate systems. Awareness of food sources becomes crucial for maintaining equilibrium.
Understanding Thyroid Disease and Autoimmunity
Millions remain unaware their daily struggles stem from malfunctioning glandular systems. Thyroid disorders often masquerade as general fatigue or stress, leaving 50% of cases undiagnosed despite clear warning signs.
Common Thyroid Disorders and Their Symptoms
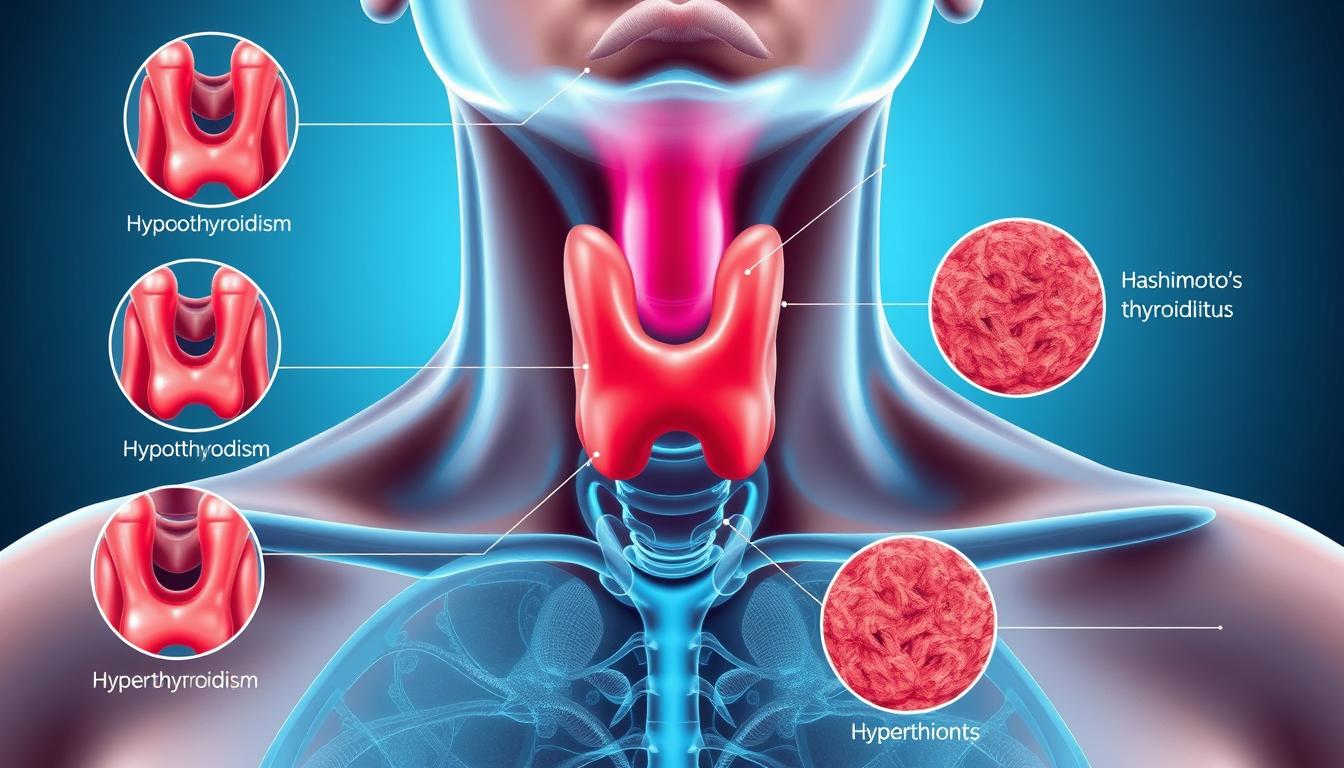
Hypothyroidism slows bodily functions like a car stuck in low gear. You might notice cold sensitivity, brittle nails, or brain fog. Weight gain often occurs despite no diet changes.
Hashimoto thyroiditis drives most underactive gland cases. This autoimmune condition tricks defenses into attacking thyroid tissue. Joint pain and hair thinning frequently accompany hormone shortages.
| Disorder | Type | Key Symptoms | Prevalence |
|---|---|---|---|
| Hypothyroidism | Hormone Deficiency | Fatigue, Weight Gain, Depression | 4.6% of U.S. Adults |
| Hashimoto’s | Autoimmune | Goiter, Muscle Weakness, Dry Skin | Women: 7x Higher Risk |
| Graves’ Disease | Autoimmune | Anxiety, Tremors, Rapid Pulse | 1.2% Population |
The Role of Autoimmunity in Thyroid Disease
Your immune system sometimes misidentifies thyroid proteins as threats. This confusion sparks chronic inflammation that gradually impairs hormone production. Women face heightened risks due to estrogen’s influence on immune responses.
Hashimoto thyroiditis progresses silently over years. Regular checkups become vital when family history includes autoimmune conditions. Early intervention prevents irreversible gland damage.
What is Gluten and Its Components
Found in countless pantry staples, this protein complex plays dual roles in nature and nutrition. Its unique properties make it both valuable for food production and challenging for human digestion.

Gluten Proteins: Gliadin and Glutenin
Two key players dominate gluten’s composition. Gliadin contributes stretchiness to dough, while glutenin provides structural strength. Together, they create the chewy texture you recognize in fresh bread.
| Protein Type | Primary Function | Digestibility | Immune Impact |
|---|---|---|---|
| Gliadin | Elasticity Creator | Low | High Reactivity |
| Glutenin | Structural Support | Moderate | Lower Reactivity |
How Gluten Is Processed in the Body
Your digestive enzymes attack gluten like puzzle solvers. Proteases break most proteins into harmless amino acids. But gluten’s complex structure resists complete breakdown.
Undigested fragments called peptides survive the journey. These remnants can slip through intestinal barriers. When detected, they may activate defense mechanisms designed to protect you.
Research shows these particles resemble certain human tissue proteins. This similarity creates potential for mistaken identity in sensitive individuals. Your protection systems sometimes attack both invaders and self-structures.
How Gluten Impacts Thyroid Function
Your body’s defense network sometimes wages war on the wrong targets. When undigested food particles slip through intestinal barriers, they can spark friendly fire against vital organs. This biological confusion creates ripple effects that disrupt hormone balance.
Molecular Mimicry and Immune Response
A healthy gut acts like a vigilant security guard. Tight junctions between intestinal cells filter nutrients while blocking harmful substances. Stress, alcohol, or medications can weaken this barrier by increasing zonulin – a protein that opens floodgates for larger particles.
When gluten fragments enter your bloodstream, immune cells sound alarms. They produce antibodies targeting gliadin, gluten’s primary protein. Research shows these defenders sometimes mistake thyroid enzymes for gluten due to nearly identical molecular patterns.
This case of mistaken identity – called molecular mimicry – explains why your antibodies might attack both invaders and gland tissue. One study found 76% of Hashimoto’s patients showed immune reactivity to gliadin. The cross-reaction creates lasting inflammation that strains hormone production.
Your immune memory holds grudges. Even after gluten leaves your system, antibodies remain on high alert for months. This prolonged vigilance keeps thyroid tissue under siege, worsening autoimmune responses over time.
Testing for Gluten-Related Thyroid Issues
Accurate diagnosis requires specialized testing that looks beyond surface-level symptoms. Modern lab evaluations can uncover hidden connections between dietary triggers and glandular dysfunction. Three key assessments help paint a complete picture of your body’s unique response patterns.
Comprehensive Thyroid and Gluten Sensitivity Panels
Your doctor may order advanced blood work to measure thyroid hormones and immune activity. Essential markers include:
| Test Type | Purpose | Key Markers | Frequency |
|---|---|---|---|
| Thyroid Panel | Assess hormone production | TSH, Free T3/T4, Antibodies | Every 6-12 months |
| Gluten Array | Detect immune reactions | Gliadin Antibodies, Tissue Transglutaminase | Initial Diagnosis |
| Celiac Screen | Confirm autoimmune response | EMA, DGP Antibodies | As needed |
Array 3X testing improves detection of non-celiac gluten intolerance by analyzing smaller protein fragments. This reduces false negatives by 40% compared to standard screens. Remember to consume gluten for six weeks before blood draws for accurate results.
The Importance of Stool and Micronutrient Testing
Gut health directly impacts nutrient absorption and immune function. Stool analysis reveals:
- Zonulin levels indicating intestinal permeability
- Microbiome diversity markers
- Digestive enzyme activity
Micronutrient panels identify deficiencies in selenium, zinc, and iron – crucial minerals for thyroid function. These tests help create personalized treatment plans addressing root causes rather than just symptoms.
Dietary Strategies for Managing Thyroid Health
Revitalizing your metabolic engine starts with strategic food choices. Elimination protocols help identify hidden triggers, with research showing 68% of participants improve symptoms within 6 weeks. Focus on anti-inflammatory foods like wild-caught fish and leafy greens to support glandular function.
Prioritize nutrient-dense meals rich in selenium and zinc. These minerals act as cofactors for hormone conversion processes. Fermented foods like kimchi strengthen gut barriers, reducing particle leakage that sparks immune confusion.
Track energy patterns after meals using a food-symptom journal. Many discover delayed reactions to common ingredients that standard allergy tests miss. Pair dietary changes with stress-reduction techniques for compounded benefits.
Work with practitioners to design personalized plans addressing root causes. Small, consistent adjustments often yield greater long-term results than drastic overhauls. Your plate becomes medicine when aligned with biological needs.