Did you know that 1 in 4 men and 1 in 10 women in the U.S. experience obstructive sleep issues? This common condition disrupts rest and impacts overall well-being. Today, advanced devices offer new ways to monitor and improve sleep quality.
Traditional methods like clinical sleep tests remain effective, but consumer-friendly wearables are gaining ground. Brands like Apple and Samsung now provide FDA-approved tracking features. These tools detect breathing disturbances with impressive accuracy.
At-home testing options also exist, combining convenience with professional-grade analysis. The choice between medical and consumer solutions depends on your needs. Comfort, cost, and validation all play key roles in finding the right fit.
Key Takeaways
- Sleep-related breathing issues affect millions of Americans
- Wearable technology now offers FDA-approved monitoring
- Professional tests provide comprehensive data for diagnosis
- Multiple factors determine the best solution for each person
- Modern devices make sleep tracking more accessible than ever
Introduction: The Battle for Better Sleep
One-third of U.S. adults now monitor their sleep with wearable devices. The $7 billion sleep tech market reflects growing awareness of sleep health as a cornerstone of wellness. From smart rings to bedside sensors, innovation is making tracking easier than ever.

Yet, 25 million Americans have undiagnosed obstructive sleep apnea (OSA). Left unchecked, it strains blood pressure and increases risk of heart disease by 140%. Studies link untreated OSA to stroke and diabetes, too.
Telemedicine bridges gaps in sleep medicine. Services like SleepTest.com offer home tests and prescription access. But the dilemma remains: Should you choose clinical-grade solutions or consumer wearables?
| Untreated OSA Risks | Likelihood Increase |
|---|---|
| Hypertension | 2.5x |
| Stroke | 1.6x |
| Type 2 Diabetes | 1.8x |
Your choice impacts daily life. Traditional methods diagnose precisely but require clinic visits. Wearables track trends but may miss severe symptoms. Understanding these trade-offs is key to restful nights.
Understanding Sleep Apnea and Snoring
Millions wake up exhausted, unaware their nighttime breathing has stopped. This could signal obstructive sleep apnea (OSA), where throat muscles collapse during sleep, blocking airflow. Unlike central sleep apnea (brain-signal issues), OSA is a physical sleep disorder.
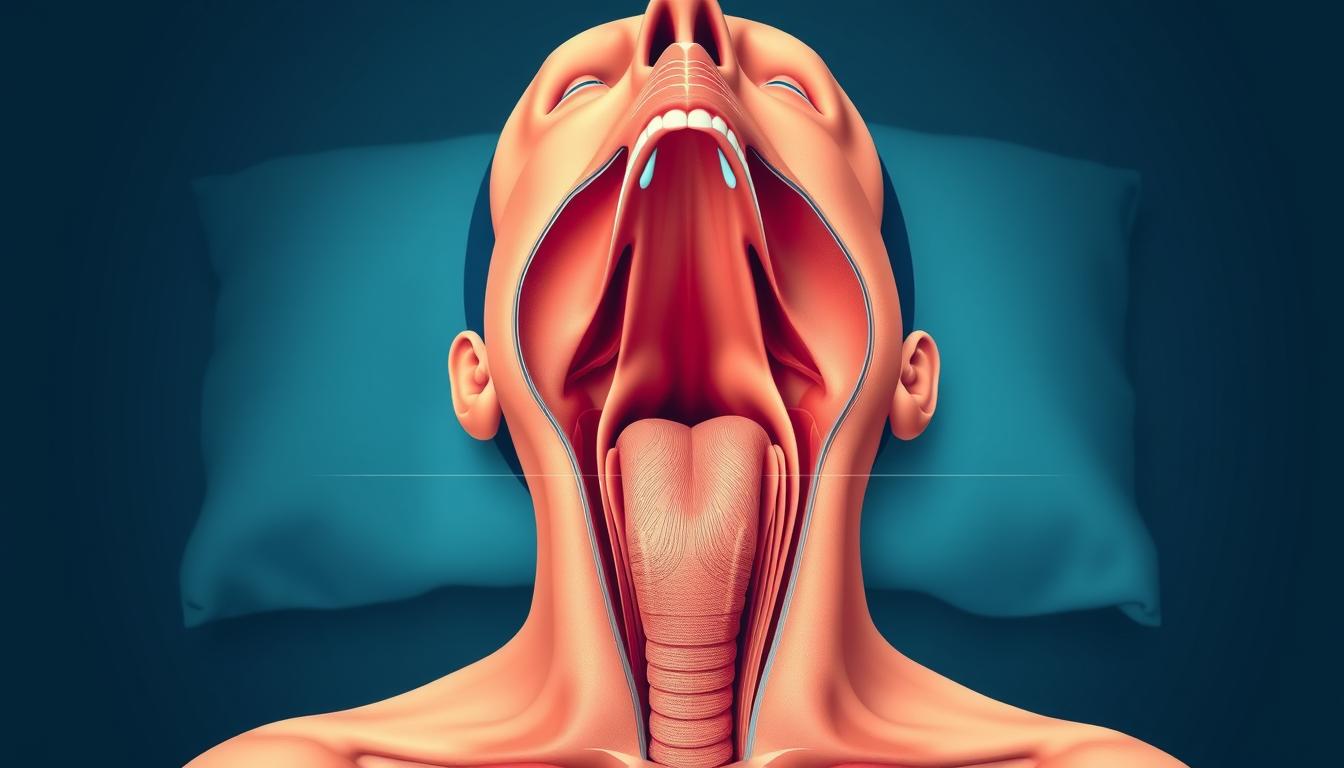
What Is Obstructive Sleep Apnea?
OSA causes repeated apneic events—pauses in breathing lasting 10+ seconds. These reduce oxygen in your blood, straining your heart. The American Academy of Sleep Medicine (AASM) notes:
“OSA severity is measured by hourly apneas. Even 5–15 events per hour demand attention.”
Untreated, these drops trigger morning headaches and chronic fatigue. Your body fights to restart breathing, fragmenting sleep.
How Snoring Relates to Sleep Disorders
Snoring happens when airways narrow, vibrating tissues. But loud snoring with gasps may indicate OSA. Here’s how sleep architecture breaks down:
| Sleep Stage | Impact of OSA |
|---|---|
| NREM (Deep Sleep) | Restorative phases shorten |
| REM | Frequent awakenings disrupt dreaming |
Healthy adults cycle through 4–5 stages each night. OSA steals deep sleep, leaving you drained. If you snore loudly and feel tired daily, consult a specialist.
Traditional Solution: How CPAP Machines Work
Continuous airflow keeps airways open—here’s how it works. CPAP (Continuous Positive Airway Pressure) delivers gentle pressure through a mask, acting like an invisible splint. This prevents throat collapses during sleep, the root cause of obstructive apnea.

The Science Behind CPAP Therapy
The treatment uses pressurized air to maintain open airways. Think of it as a cushion that stops tissues from sagging. Clinicians call this pneumatic splinting.
Your exact pressure needs are determined through a process called titration. During a sleep study, technicians adjust levels until breathing stabilizes. Some kits now allow home titration for convenience.
Who Benefits Most from CPAP?
Ideal candidates include those with:
- Moderate-to-severe apnea (15+ hourly events)
- Daytime fatigue despite long sleep
- High blood pressure linked to poor rest
Medicare and insurers often cover CPAP after a formal diagnosis. However, 40% of users struggle with initial mask discomfort. Most adapt within weeks as sleep quality improves.
Modern Alternatives: The Rise of Smart Wearables
Your wrist could now hold the key to detecting sleep apnea. Leading tech companies have developed wearable devices that monitor breathing patterns overnight. These tools make sleep tracking more accessible than traditional methods.

Apple Watch’s Sleep Apnea Detection
The Apple Watch analyzes 30 days of breathing patterns to spot disturbances. It uses photoplethysmography (PPG) to measure blood flow changes at your wrist. Results show as “elevated” or “not elevated” rather than medical diagnoses.
Key features include:
- Nightly breathing rate monitoring
- Movement detection during sleep
- FDA-cleared (not approved) as a wellness tool
Samsung’s FDA-Approved Sleep Tracking
Samsung’s technology requires just two nights of tracking (4+ hours each) within 10 days. It combines PPG with accelerometers to track movements. The system has age restrictions—it only works for users 22+ years old.
Both devices:
- Share data easily with healthcare providers
- Offer trend analysis over time
- Complement but don’t replace medical sleep studies
While convenient, remember these wearables provide screening—not diagnosis. Their sleep apnea detection capabilities help identify when to seek professional evaluation.
Snore Tech Showdown: CPAP vs. Smart Wearables
Choosing the right sleep solution depends on balancing accuracy with comfort. While clinical-grade tools diagnose sleep disorders precisely, wearables excel in convenience. Understanding these trade-offs helps you pick the best fit.

Effectiveness in Apnea Detection
Polysomnography (PSG) detects 98% of apneas—the gold standard for accuracy. The best wearables, like FDA-cleared models, catch 85%. Key differences:
- AHI measurement: Clinical tests track apnea-hypopnea index (AHI) with sensors on your chest and face. Wearables estimate it via wrist movements.
- Validation levels: PSG meets CMS requirements for diagnosis. Wearables are FDA-cleared for screening only.
- Proven efficacy: CPAP reduces AHI by 90% in trials. Wearables monitor sleep stages but don’t treat apnea.
Comfort and Usability Compared
Here’s how nightly routines differ:
- Setup time: CPAP requires 15 minutes for mask fitting and humidifier prep. Wearables need zero prep—just wear them.
- Sleep positions: CPAP masks may shift during movement. Watches stay put but can’t track quality during side sleeping.
- Long-term use: 60% of users adapt to CPAP within a month. Wearables face fewer compliance issues but lack therapeutic benefits.
Accuracy Face-Off: Wearables vs. Clinical Sleep Studies
Modern sleep tracking has evolved dramatically, but how accurate are these new methods? While wearables offer convenience, clinical-grade sleep study tools like polysomnography (PSG) remain the gold standard. Understanding their differences helps you interpret results correctly.
How Wearables Measure Up to Polysomnography
PSG uses 7+ sensors to track brain waves, eye movements, and muscle activity. Wearables rely on just 2-3 sensors—usually PPG and accelerometers. This table shows key contrasts:
| Measurement Type | Clinical PSG | Consumer Wearables |
|---|---|---|
| Brain Activity | EEG Sensors | Not Measured |
| Breathing Patterns | Chest Belts + Nasal Cannula | PPG (Wrist Blood Flow) |
| Movement Detection | EMG Sensors | Accelerometer Only |
The American Academy Sleep Medicine cautions:
“Wearables may miss 20% of apnea events due to motion artifacts and limited sensor arrays.”
When CPAP Still Reigns Supreme
Severe OSA cases require PSG confirmation. Hybrid devices like WatchPAT 300 improve accuracy (89%) by adding peripheral arterial tone (PAT) and SpO2 sensors. Yet expert consensus agrees:
- Wearables excel at trend tracking, not diagnosis
- False negatives occur during side sleeping
- Clinical tests detect central apnea, which wearables often miss
These limitations matter most if you gasp awake frequently. For mild symptoms, wearables provide useful screening. But persistent fatigue warrants a lab sleep study.
Convenience and Lifestyle Fit
Your daily routine impacts which sleep solution fits best. Some prioritize clinical precision, while others need flexibility. Here’s how home setups and portable devices compare for real-world use.

CPAP’s Home Setup Challenges
Traditional machines require more than just plugging in. You’ll need:
- Distilled water for humidifiers (tap water causes mineral buildup)
- Monthly filter replacements to maintain air quality
- Power outlets nearby—camping or outages pose problems
Noise levels vary by model. Some hum softly, while others distract light sleepers. Travel adds complexity—hotels may lack bedside tables for equipment.
Wearables: Sleep Tracking On the Go
Smart rings and watches simplify routines. The Oura Ring adjusts to time zones automatically, ideal for frequent flyers. Key perks:
- No setup—wear it and forget it
- Charges via USB (unlike CPAP’s power brick)
- Silent operation won’t disturb partners
Data syncs wirelessly to apps, letting you spot trends. But remember: These devices track—they don’t treat apnea.
Cost Comparison: Upfront and Long-Term
Budget considerations play a crucial role in selecting sleep solutions. Whether you choose medical-grade treatment or consumer wearables, expenses vary significantly over time. Understanding these differences helps you plan for better sleep without financial surprises.

Insurance Coverage for CPAP
Most health plans cover 80% of CPAP costs after meeting your deductible. Medicare follows specific rules:
- Rentals for 13 months before ownership transfers
- Requires proof of 4+ hours nightly use for compliance
- Covers masks, tubing, and filters as durable medical equipment
The process involves a sleep study prescription and supplier accreditation checks. Out-of-pocket costs typically range from $250-$800 annually after insurance.
Subscription Models in Wearable Tech
Smart devices often use recurring fees for advanced features. Popular options include:
- Oura Ring: $6/month for sleep staging analytics
- Whoop 4.0: $30/month with free hardware
- Apple Watch: One-time $399+ purchase with optional health apps
These services provide cloud storage and personalized insights. Unlike CPAP, they don’t qualify for insurance reimbursement.
| Solution | First-Year Cost | 5-Year Total |
|---|---|---|
| CPAP (With Insurance) | $500-$1,200 | $2,100-$3,800 |
| Premium Wearable + Subscriptions | $429-$699 | $1,700-$2,500 |
Your health needs and budget determine the smarter investment. While CPAP has higher initial cost, wearables accumulate fees over time. Consider both financial and therapeutic benefits when choosing.
User Experience: Nightly Routine Adaptations
Adapting to new sleep solutions takes time—here’s what to expect. Whether you choose clinical-grade therapy or consumer devices, your user experience impacts long-term success. Nearly 40% abandon traditional options within a year due to comfort challenges.

The CPAP Adjustment Period
Clinical solutions require patience. Nasal masks need precise fitting—too tight causes pressure marks, too loose leaks air. Most users cycle through 2-3 mask types before finding the right seal.
Humidifiers add complexity. You’ll learn to:
- Adjust water levels for ideal moisture
- Clean tanks daily to prevent bacteria
- Manage condensation in tubing
Hose management becomes a nightly ritual. Some drape it overhead, while others use bedside clips. Average adaptation takes 2-8 weeks, with sleep quality improving gradually.
Wearables: Plug-and-Play Simplicity
Consumer devices work immediately. Fitbit and Apple Watch start tracking when you fall asleep—no buttons to press. Their automatic operation eliminates setup stress.
Key advantages include:
- Zero maintenance beyond charging
- No partner disturbance from noise
- Data syncs wirelessly by morning
While convenient, remember these trackers don’t treat breathing issues. They’re ideal for spotting trends but won’t stop apnea events during the night.
Your choice depends on sleep needs. Those with severe symptoms endure CPAP’s learning curve for therapy. Mild cases may prefer wearables’ hassle-free monitoring.
Expert Opinions on Tech-Driven Solutions
Medical professionals weigh in on the accuracy of sleep-tracking innovations. While consumer devices gain popularity, clinicians emphasize critical differences between monitoring and medical diagnosis. Their insights help navigate claims about detecting breathing disruptions during sleep.
What Sleep Specialists Say
Dr. Weidenbecher of Unity Health Network states clearly: “Wearables can’t replace PSG for diagnosing sleep apnea.” The American Academy of Sleep Medicine (AASM) supports this position:
“Consumer devices may miss 30% of apnea events in patients with high blood pressure risks. Clinical confirmation remains essential for treatment plans.”
Key limitations noted by specialists:
- Movement artifacts distort oxygen level readings
- No measurement of brain wave disruptions
- False positives create unnecessary patient anxiety
Current protocols still require in-lab testing for prescriptions. This ensures proper assessment of your sleep disorder severity before therapy begins.
FDA’s Role in Validating Devices
The FDA cleared Samsung’s sleep monitoring app as a De Novo device—a classification for novel technologies. This differs from traditional 510(k) clearance for established medical equivalents.
| Clearance Type | Requirements | Intended Use |
|---|---|---|
| 510(k) | Proves equivalence to existing devices | Diagnosis and treatment |
| De Novo | Demonstrates safety for new technology | Screening and tracking |
This distinction matters when choosing solutions. Cleared devices meet baseline safety standards but aren’t approved to diagnose sleep apnea independently. Always discuss abnormal results with a sleep specialist.
Limitations of Wearable Sleep Tech
Not all sleep disruptions can be detected by wrist-worn devices. While convenient, these tools have significant limitations in tracking breathing disorders. Understanding these gaps helps you interpret your sleep data more accurately.
False Alarms and Data Gaps
Stanford researchers found the Oura Ring misses 22% of apnea events. This occurs because photoplethysmography (PPG) sensors lose signal during movement. When you roll over, the device may record false normal breathing.
Other common issues include:
- No oxygen level tracking (SpO2 sensors excluded in most models)
- BMI over 30 may distort optical sensor readings
- Atrial fibrillation creates interference patterns

Age and Health Restrictions
Most wearables aren’t designed for children, despite 1-4% having pediatric OSA. Samsung’s FDA-cleared app specifically excludes users under 22. Those with pre-existing conditions face additional problems.
Key restrictions:
- Not recommended for arrhythmia patients
- Limited validation for seniors over 70
- Pregnancy-related breathing changes aren’t accounted for
These age and health factors mean wearables work best for generally healthy adults. Always consult a doctor if your device shows concerning patterns.
CPAP’s Drawbacks You Should Know
Effective as it may be, CPAP treatment isn’t without its drawbacks. While clinically proven to reduce apnea events, users frequently report challenges that impact comfort and consistency. Understanding these issues helps you prepare for the adjustment period.
Common Complaints from Users
Three issues dominate CPAP user feedback:
- Mask leaks: 45% experience air escaping, causing dry eyes or disrupted sleep
- Noise levels: While quieter than older models, some machines hum at 30 decibels
- Claustrophobia: First-time wearers often need weeks to adapt to facial contact
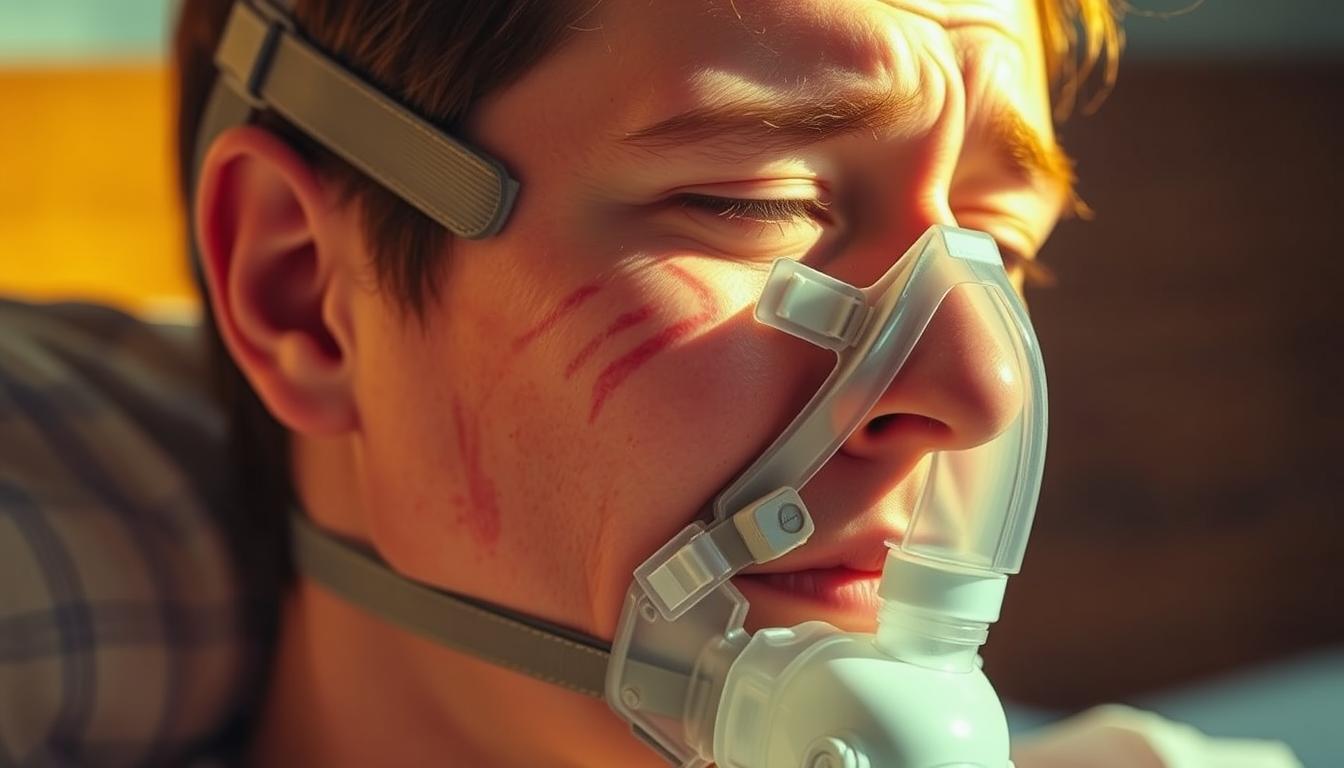
Dry mouth affects 30% of users, especially those breathing through their mouths. Heated humidifiers help but require nightly refilling. Partner quality of sleep may suffer too—40% report disturbance from machine sounds or tubing movement.
Maintenance and Cleaning Hassles
CPAP demands rigorous hygiene to prevent bacterial growth. The daily process includes:
- Washing masks with mild soap
- Emptying and drying humidifier chambers
- Weekly filter replacements (monthly for hypoallergenic filters)
Travel introduces extra considerations. You’ll need:
- Portable battery packs for flights/camping
- Compact travel machines (often not insurance-covered)
- Distilled water sources at destinations
APAP machines (auto-adjusting pressure) require less manual tuning but share these maintenance needs. Without proper care, pneumonia risk increases by 32% according to clinical studies.
Despite these challenges, most users find the fatigue relief outweighs the hassles. Giving yourself 2-3 months to adapt significantly improves long-term success rates.
Future Trends in Sleep Apnea Management
The next generation of sleep solutions blends cutting-edge technology with personalized care. From AI-driven diagnostics to hybrid devices, innovations aim to make detection and treatment more precise and accessible. These advancements promise to transform how we understand and address nighttime breathing disruptions.

AI and Predictive Analytics
Machine learning now powers devices like the Dreem Headband, which analyzes EEG data to map sleep architecture. Unlike traditional methods, these tools spot subtle patterns humans might miss. ResMed’s AirSense 11 takes it further—it auto-adjusts pressure levels in real time based on your breathing.
Emerging developments include:
- Raw PPG analysis that detects apnea without clinical sensors
- Predictive algorithms flagging risk factors before symptoms appear
- Cloud-based platforms that compare your metrics against population health trends
“Deep learning models will soon predict apnea episodes 30 minutes before they occur, allowing preemptive intervention.”
Hybrid Solutions on the Horizon
The future lies in merging clinical-grade accuracy with wearable convenience. Startups like SleepImage combine ring sensors with SaaS analytics—your doctor receives detailed reports without lab visits. Meanwhile, implantable sensors are being tested for severe cases.
| Innovation | Function | Availability |
|---|---|---|
| Smart CPAP Masks | Sync with wearables to monitor sleep stages | 2025 (FDA pending) |
| Contactless Bed Sensors | Track breathing via radar technology | Currently in trials |
| Genetic Risk Profiles | DNA testing for apnea predisposition | 2024 pilot programs |
Insurance coverage may soon expand for these hybrid devices. Medicare is evaluating reimbursement for combined diagnostic-therapeutic systems. As validation grows, expect more options bridging home convenience with medical precision.
How to Choose the Right Option for You
Finding the best sleep solution starts with understanding your unique needs. Your sleep disorder severity and daily habits both play crucial roles. This decision framework helps match your situation with effective options.
Assessing Your Sleep Apnea Severity
The STOP-BANG questionnaire quickly screens risk factors. Score one point for each:
- Snoring loud enough to hear through doors
- Daytime tiredness despite full nights in bed
- Observed breathing pauses during sleep
- Blood pressure over 140/90 mmHg
Scores of 3+ suggest moderate-to-severe apnea needing clinical sleep apnea diagnosis. Match your results to these treatment tiers:
| AHI Score | Recommended Approach |
|---|---|
| 5-15 (Mild) | Lifestyle changes + wearables |
| 15-30 (Moderate) | Oral appliances or APAP trial |
| 30+ (Severe) | CPAP with clinical oversight |
Lifestyle Factors to Consider
Frequent travelers face different challenges than homebodies. Portable solutions work best if you:
- Spend 10+ nights monthly in hotels
- Need TSA-friendly equipment
- Lack reliable power sources
Weight loss impacts OSA management. Research shows:
“Every 10% body weight reduction decreases AHI by 26% in obese patients.”
Mild cases may try step-up approaches. Start with positional therapy and track symptoms for 4-6 weeks. If fatigue persists, consult an expert for advanced testing.
Conclusion: Finding Your Path to Quiet Nights
Restful nights begin with the right approach to your sleep health. While wearables help spot patterns, they can’t replace a professional diagnosis. Clinical tests remain essential for accurate results.
For best outcomes, combine tools. Use tracking devices to monitor trends and consult specialists for treatment plans. Studies show coached users adapt 68% better to therapies.
Start with these steps:
- Try home test kits if lab visits aren’t feasible
- Share wearable data with your doctor
- Prioritize comfort alongside clinical efficacy
Your sleep quality improves when technology and expertise work together. Take action today—your healthier tomorrow starts tonight.