Did you know 70% of your immune system is in your digestive tract? Yale researchers found this out. They say intestinal balance might solve autoimmune puzzles. A study showed that Enterococcus gallinarum, a common gut bacterium, can get into the blood of some people.
Once in the blood, it causes inflammation like lupus. This happens because of molecular mimicry.
Your gut lining is like a security checkpoint. It’s controlled by proteins like zonulin. If this system fails, food and microbes can leak into your blood. Your immune system then attacks these as enemies, sometimes mistaking them for your own cells.
This is why diseases like rheumatoid arthritis and Hashimoto’s thyroiditis often go with digestive problems.
New research links what you eat to zonulin levels. Foods with gluten or additives can weaken your gut over time. But foods like kimchi and kefir can boost your gut health. Knowing this lets you make better choices about what you eat and how you live.
Key Takeaways
- Yale research identifies specific gut bacteria that trigger autoimmune responses
- Molecular mimicry causes immune confusion between microbes and human tissues
- Zonulin proteins regulate intestinal permeability like gatekeepers
- Diet directly impacts gut barrier integrity within weeks
- 70% of immune activity originates in digestive system tissues
Understanding the Gut-Immune System Connection
Your gut does more than just digest food. It plays a key role in your body’s defense. Almost 80% of your immune cells live in your gut walls. This makes your gut a fast-acting defense center.
This partnership has evolved over thousands of years. It turns your digestive tract into a sophisticated security checkpoint.
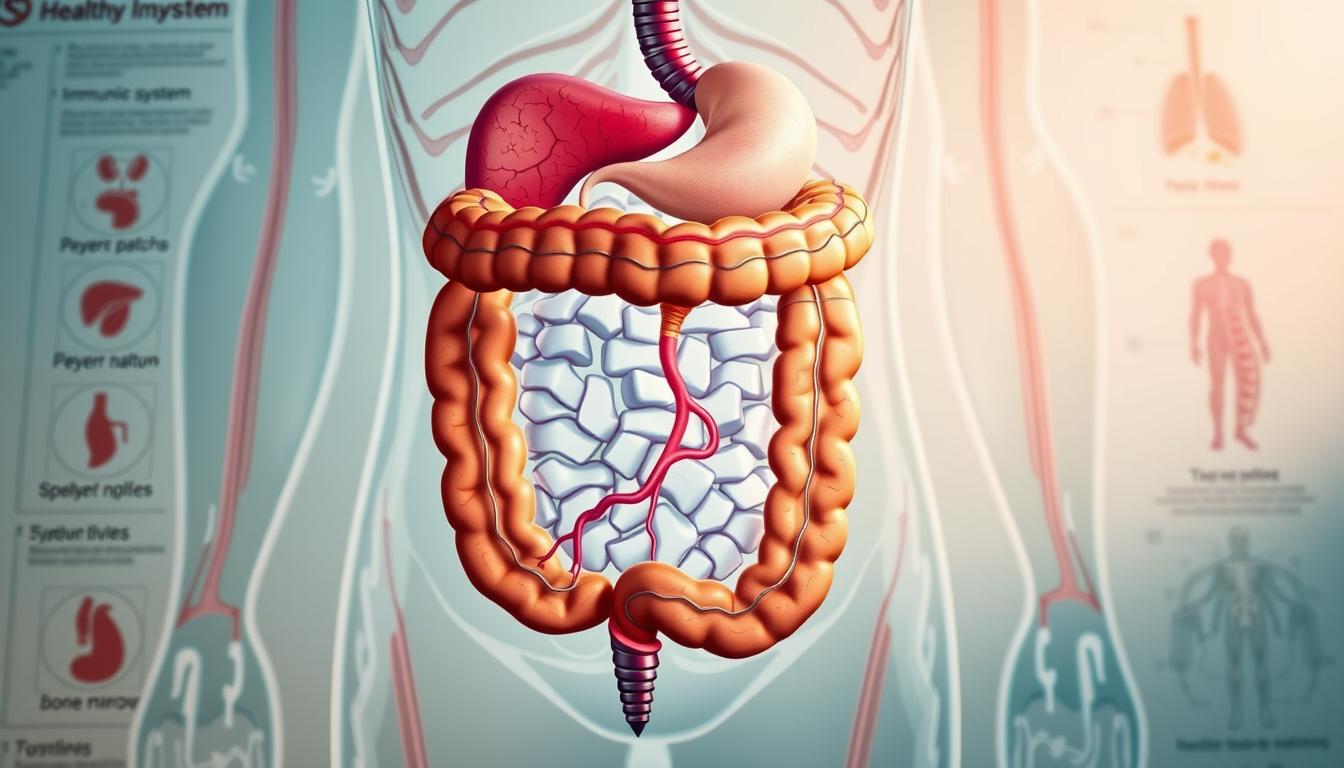
Your Second Brain: How Gut Function Impacts Immunity
The gut-associated lymphoid tissue (GALT) is your body’s largest immune training camp. This network:
- Scans 60 tons of food across an average lifetime
- Houses more antibodies than any other organ
- Directs immune responses through cytokine signaling
Gut-Associated Lymphoid Tissue (GALT) Explained
Your GALT has Peyer’s patches – immune monitoring stations. These stations use M-cells to:
- Detect harmful pathogens
- Trigger targeted antibody production
- Store immune memory cells
Microbiome’s Role in Immune Cell Training
Beneficial bacteria train your immune system. They:
- Teach T-cells to distinguish friend from foe
- Produce short-chain fatty acids that regulate inflammation
- Compete with harmful microbes for resources
“The microbiome doesn’t just influence immunity – it fundamentally rewires immune responses through epigenetic changes,” notes Dr. Ana Kriegel’s 2023 leaky gut study.
The Leaky Gut Phenomenon
When your gut barriers fail, harmful substances enter your bloodstream. Modern tests use fecal calprotectin levels to measure this. Levels above 50 mcg/g often show a compromised barrier.
Intestinal Permeability Mechanisms
Tight junctions between gut cells act like Velcro® strips. Factors that weaken these bonds include:
- Chronic stress hormones
- NSAID pain relievers
- Gluten-derived peptides
Zonulin Protein’s Crucial Role
This protein controls gate openings in your gut lining. High zonulin levels:
- Increase barrier permeability within 15 minutes
- Trigger inflammatory cascades
- Correlate with autoimmune antibody production
Recent studies show 25% higher zonulin levels in patients with multiple autoimmune conditions compared to healthy controls.
The Hidden Link Between Gut Health and Autoimmune Disorders Revealed
Research is showing how gut bacteria might harm your immune system. It’s found that gut health and autoimmunity are linked. This could change how we fight chronic diseases.
Molecular Mimicry Mechanisms
Your immune system might confuse good gut bacteria with threats. This case of mistaken identity happens when bacteria proteins look like human tissues. Yale researchers found that E. gallinarum bacteria have proteins very similar to human joint proteins.
Case study: Rheumatoid arthritis and gut bacteria
A 2022 study found that rheumatoid arthritis patients had 80% higher Prevotella copri levels than healthy people. These bacteria have proteins that look like collagen in your joints. This can lead to your immune system attacking your joints by mistake.
“The evolutionary arms race between humans and microbes has left dangerous similarities in protein structures,” notes Dr. Palm’s genomic analysis.
Dysbiosis Patterns in Autoimmune Patients
Almost all autoimmune diseases have unique gut microbiome imbalances. These imbalances are not just about “good” vs “bad” bacteria. They show complex disruptions in the ecosystem:
- Firmicutes/Bacteroidetes ratio: Usually different from healthy people
- Akkermansia muciniphila: Often 40-60% lower
- Proteobacteria overgrowth: Linked to inflammation in the intestines
Common microbial imbalances identified
Studies found three key markers in autoimmune patients:
- Less butyrate-producing species (Roseburia, Faecalibacterium)
- More LPS-containing bacteria (Enterobacteriaceae)
- Missing key species that help with immune tolerance
These imbalances create a perfect storm for autoimmune diseases. Your gut lining gets more permeable. Inflammatory compounds keep challenging your immune system. The next section will look at specific conditions linked to these gut-immune issues.
Autoimmune Conditions Linked to Gut Health
Did you know your gut health could play a big role in autoimmune diseases? Research shows certain digestive system imbalances can trigger or make conditions like Crohn’s disease and lupus worse. Let’s dive into how these connections affect managing autoimmune diseases.
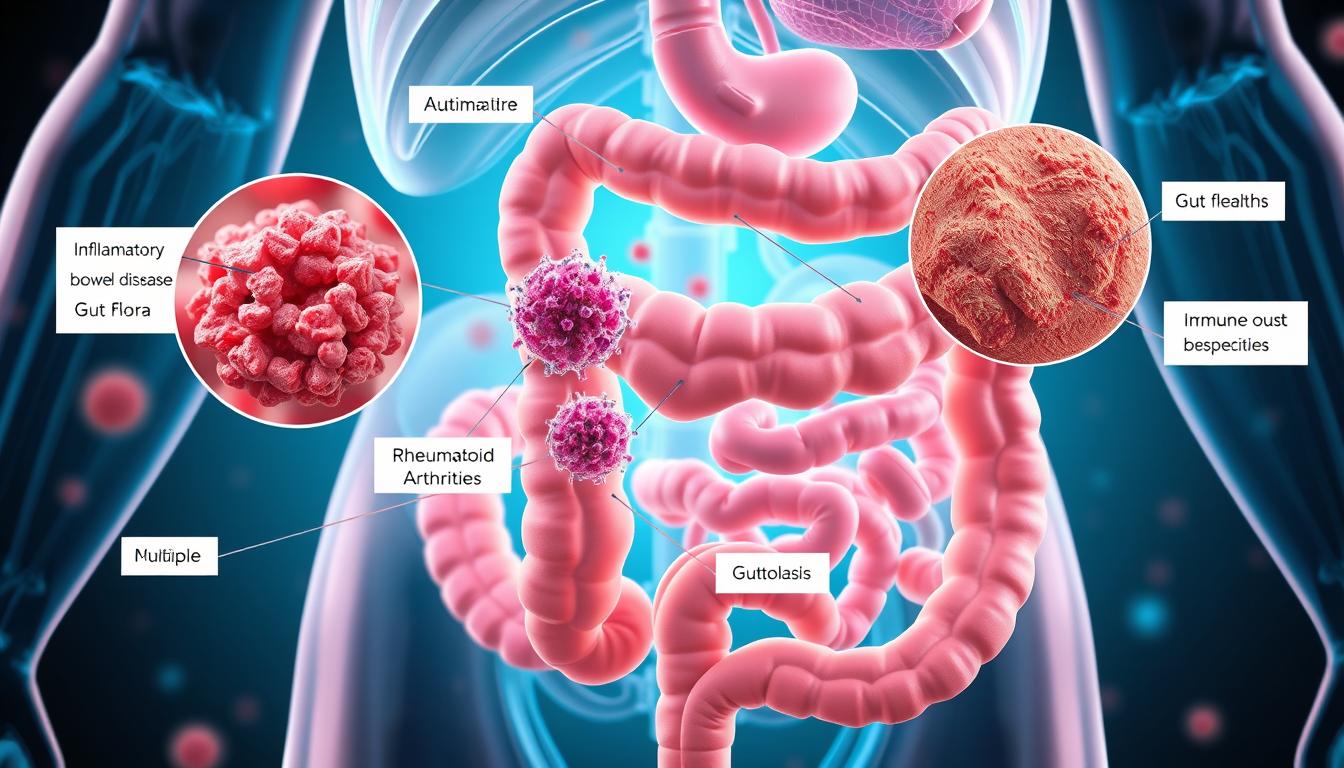
Inflammatory Bowel Diseases
Your gut microbiome is like a fingerprint for autoimmune risks. In Crohn’s disease, scientists have found unique bacterial patterns that are different from healthy people.
Crohn’s Disease Microbiome Signatures
Faecalibacterium prausnitzii, a good gut bacteria, is often low in Crohn’s patients. It helps reduce inflammation and strengthen the gut lining. Without it, harmful bacteria can cause immune overreactions.
Ulcerative Colitis Treatment Breakthroughs
2023 clinical trials showed promising results for ulcerative colitis treatment. Fecal microbiota transplants (FMT) helped patients:
- Reduce flare-ups by 53%
- Improve mucus layer regeneration
- Respond better to conventional medications
Non-Digestive System Disorders
The gut-autoimmune connection isn’t just for bowel diseases. New evidence shows microbial imbalances can affect your brain, joints, and skin.
Multiple Sclerosis Gut Connection
Specific gut bacteria produce compounds that can reach the nervous system. These compounds might mistakenly activate immune cells that attack myelin. Researchers found MS patients often have:
- Higher levels of methane-producing bacteria
- Lower diversity in core microbiome strains
Lupus and Intestinal Permeability
A study led by Dr. Martin Kriegel found Enterococcus gallinarum in 83% of lupus patients’ livers, compared to 0% in healthy controls. This bacterial translocation happens through leaky gut barriers, leading to chronic inflammation and autoimmune attacks.
Modern Science’s Perspective
New discoveries are changing how we see the link between our gut and immune system. Studies are finding patterns in microbes that could lead to new treatments for autoimmune diseases.
Latest Research Findings (2020-2023)
Fecal Microbiota Transplantation Results
In 2023, trials showed fecal transplants helped 58% of patients with inflammatory bowel disease. But, there are some downsides:
- 20% of patients had temporary bloating or cramping
- 5% faced risks of antibiotic-resistant infections
- Most effects lasted 6-18 months

Yale researchers stunned the world with their E. gallinarum study. This gut bacterium acts differently in people with autoimmune diseases. It makes proteins that confuse immune cells. Dr. Palm’s team found these changes happen before symptoms appear in 67% of cases.
Controversies in Medical Community
Chicken-or-Egg Debate: Gut vs Immunity
Experts disagree on which system fails first. Boston immunologists say:
“Immune dysfunction creates the environment for microbial imbalance, not the reverse.”
But gut specialists argue with data showing:
- 94% of lupus patients have abnormal gut permeability
- 72% show microbiome changes 2+ years before diagnosis
The use of immunosuppressants adds to the debate. These drugs may reduce inflammation but also:
- Deplete beneficial bacteria
- Increase pathogenic species
- Lead to long-term dependency risks
Dietary Factors That Influence Both Systems
What you eat affects your digestive system and immune defenses. Research shows that some foods help or harm this balance. We’ll look at foods that disrupt harmony and how to eat better to restore it.
Problematic Food Components
Some proteins and sugars can upset your gut and immune system. Knowing which foods to avoid is the first step to healing.
Gluten’s Dual Impact on Gut and Immunity
Gluten in wheat increases zonulin, which loosens gut cells. This creates gaps for undigested food to get into your blood. Your immune system then fights these invaders, which can harm your own tissues.
Dairy Protein Controversies
Casein in dairy is similar to gluten and can confuse your immune system. A 2023 study found 62% of autoimmune patients had antibodies against casein. While fermented dairy like kefir may help some, others need to avoid it during flare-ups.
“Our data shows symptom reduction in 73% of participants following strict elimination of immunogenic foods for 90 days.”
Healing Nutritional Approaches
Making smart food choices can calm your immune system and fix your gut. These methods are backed by science and easy to follow.
Autoimmune Protocol (AIP) Diet Basics
This diet removes common triggers for 4-6 weeks, then adds foods back slowly. Key points include:
- Eating collagen-rich bone broth
- Choosing omega-3s from wild-caught fish
- Using anti-inflammatory herbs like turmeric
FODMAP Modification Strategies
For those with SIBO, cutting down on fermentable carbs helps. New guidelines suggest:
- Eating most carbs before 3 PM
- Pairing high-FODMAP foods with digestive enzymes
- Trying 12-hour overnight fasts
Eating with your body’s natural rhythms improves nutrient absorption and reduces inflammation. Start with small changes, like eating dinner 3 hours before bed. This simple shift can boost microbial diversity by 18%, studies show.
Probiotics and Autoimmunity
Probiotics might seem small, but they can have a big impact on autoimmune conditions. They work by targeting specific areas in the body. Some probiotics can calm inflammation, while others might make it worse. Choosing the right probiotics is key to balancing gut health and autoimmunity.

Strain-Specific Therapeutic Effects
Not all probiotics are created equal. Research shows that certain strains can target specific immune responses:
Lactobacillus casei for Rheumatoid Arthritis
A 2022 Yale study found that Lactobacillus casei Shirota reduced inflammation in arthritis patients. The benefits were:
- CRP levels dropped from 8.2 mg/L to 4.9 mg/L
- Morning stiffness decreased by 35%
- Fewer gastrointestinal side effects than standard NSAIDs
| Strain | Autoimmune Condition | Observed Effect |
|---|---|---|
| Bifidobacterium infantis | Hashimoto’s thyroiditis | Reduced TPO antibodies by 22% |
| Saccharomyces boulardii | Crohn’s disease | Decreased relapse rate by 31% |
| Lactobacillus rhamnosus | Multiple sclerosis | Improved gut barrier function |
Potential Risks of Supplementation
Probiotics are not without risks. About 15% of autoimmune patients may experience worsened symptoms from the wrong strains.
When Probiotics Might Worsen Symptoms
Strains like Lactobacillus casei and Lactobacillus reuteri can cause problems in sensitive people. Look out for:
- Unexplained skin rashes
- Sudden fatigue after supplementation
- Increased joint pain
| Risk Factor | Safe Alternative | Action Step |
|---|---|---|
| High-histamine strains | Bifidobacterium longum | Check strain histamine profile |
| Immunosuppressant use | Separate intake by 3+ hours | Consult prescribing physician |
| SIBO diagnosis | Soil-based probiotics | Confirm with breath test first |
“2023 clinical guidelines recommend spacing probiotics 3 hours apart from immunosuppressants to prevent reduced efficacy of both treatments.”
Stress-Gut-Autoimmunity Triangle
Stress doesn’t just affect your mood. It also changes your gut and immune system. This creates a cycle where stress makes your gut leaky, leading to autoimmune issues. Let’s explore how stress and mindfulness impact this balance.
Cortisol’s Double-Edged Sword
Short-term stress boosts secretory IgA (sIgA) in your gut. This helps fight off bad guys. But long-term stress has the opposite effect. A 2023 review found:
- Chronic cortisol lowers sIgA by 38%
- It increases gut leakiness by 2.1x
- Changes gut bacteria in just 7 days
HPA Axis Dysregulation Effects
When your HPA axis is always on, it messes with your gut. This can lead to:
| Cortisol Type | Gut Impact | Immune Effect |
|---|---|---|
| Acute (Short-Term) | Boosts sIgA production | Temporary immune activation |
| Chronic (Long-Term) | Reduces mucosal repair | Sustained inflammation |
Mind-Body Interventions
To break the stress-gut cycle, we need to change how our nervous system reacts. A 2023 UCLA study found daily meditation:
- Lowered zonulin (leaky gut marker) by 29% in 8 weeks
- Increased Bifidobacterium levels
- Improved pain in rheumatoid arthritis patients
Meditation’s Measurable Gut Impacts
Meditation boosts gut-brain connection through the vagus nerve:
- Diaphragmatic breathing (5 minutes twice daily)
- Guided imagery focusing on abdominal warmth
- Yoga poses that compress/release digestive organs
People using these methods had 40% fewer autoimmune flare-ups in recent studies.
Diagnostic Approaches
Finding gut imbalances needs advanced tests, especially for those with autoimmune diseases. These tests go beyond simple stool tests. They give deep insights into the gut’s health, how well it works, and how it interacts with the immune system. This helps find out how your microbiome and autoimmune disorders are connected.

Comprehensive Stool Analysis
Stool tests today offer key details about gut health. They are more than basic tests. They check:
Key markers to request from your doctor
- Beta-defensin 2: Shows how well the gut lining fights off microbes
- Secretory IgA: Tells us how active the immune system is
- Calprotectin: Points to inflammation in the intestines
- Zonulin family peptides: Shows if the gut is leaking
| Test Type | Technology | Key Markers | Best For |
|---|---|---|---|
| LC/MS Stool Test | Liquid chromatography-mass spectrometry | Beta-defensin 2, Fatty acids | Metabolic byproducts analysis |
| PCR Stool Test | Polymerase chain reaction | Bacterial DNA, Pathogens | Microbial identification |
Intestinal Permeability Testing
Testing for leaky gut has gotten much better. Old tests like the lactulose/mannitol test are still used, but new serum zonulin tests are more accurate. Blood tests are better than urine tests for many reasons.
Lactulose/mannitol test limitations
- Dietary sugars can skew results
- Kidney function affects excretion rates
- Hydration levels alter concentration measurements
For those with autoimmune diseases, combining stool tests with serum zonulin tests is best. This method clearly shows how microbiome changes affect gut barrier function during treatment.
Pharmaceutical Considerations
Your medicines might be harming your gut health instead of helping it. Many drugs for autoimmune diseases can upset your digestive system’s balance. This can make symptoms worse over time. Knowing how these drugs interact with your gut is key to making better choices with your doctor.
PPI Medications Hidden Dangers
Proton pump inhibitors (PPIs) like omeprazole help with heartburn by reducing stomach acid. But, long-term use has hidden risks. A 2023 study found these drugs increase Enterococcus bacteria by 300%.
This bacteria is linked to inflammation. Without enough stomach acid, harmful microbes can live in your gut.
Long-term acid suppression risks
People taking PPIs for a long time often have more bacteria in their small intestines. They also get less magnesium and B12. This weakens their immune system and can lead to more autoimmune problems.
It also hides the real problems in your digestive system.
Immunosuppressant-Gut Interactions
Drugs like methotrexate calm an overactive immune system. But, they kill off good gut bacteria. Studies show a 65% drop in important bacteria within 8 weeks.
This loss can make gut problems worse, even if the disease is controlled.
Methotrexate microbiome effects
New guidelines suggest taking probiotics at least 4 hours apart from methotrexate. This helps keep more good bacteria in your gut. Clinical trials show it keeps 30% more diversity in your gut.
“Always coordinate supplement use with biologic medications – mismatched timing can reduce treatment efficacy by up to 50%.”
Work with your doctor to find the right balance. Simple changes like staggered dosing or specific probiotics can help. These adjustments can make your medications work better for managing autoimmune diseases long-term.
Lifestyle Modifications
Your daily habits have a big impact on your gut and immune system. While diet is important, sleep and toxins also play a big role. Let’s look at ways to improve these areas.
Sleep Quality Optimization
Poor sleep can harm your gut microbiome. Studies show that melatonin helps Akkermansia muciniphila, a key gut bacteria. Without good sleep, this bacteria decreases, leading to immune issues.
Circadian Rhythm Entrainment Techniques
- Get 10 minutes of morning sunlight within 30 minutes of waking
- Stop blue light exposure after 8 PM using screen filters or amber glasses
- Keep bedtime consistent (±20 minutes) even on weekends
“Nightshift workers show 37% lower Akkermansia levels compared to day workers—a gap linked to melatonin disruption.”
Environmental Toxin Reduction
Many chemicals harm your gut lining. Bisphenol-A (BPA) is especially bad, damaging your gut at very low levels. These levels are often found in blood tests.
BPA and Gut Lining Damage
Use glass or stainless steel instead of plastic for food. Thermal receipts have a lot of BPA—wash your hands after touching them. BPA-free labels don’t always mean it’s safe; some substitutes can also harm your gut.
Key Takeaway: Good sleep and avoiding toxins help your gut and immune system. Keep track of your progress with journals and tests every 3-6 months.
Emerging Therapies
New treatments are changing how we fight autoimmune diseases. They focus on two main areas: boosting microbial byproducts and fixing gut ecosystems with microbial transfers.
Postbiotic Supplements
Butyrate, a gut bacteria product, is being studied for its anti-inflammatory powers. In 2023, studies showed it helped 22% of IBD patients get better in 12 weeks. It works by:
- Strengthening intestinal barrier function
- Regulating immune cell activity
- Reducing inflammatory cytokine production
Butyrate Supplementation Research
Now, Phase III studies are looking at timed-release butyrate to better reach the colon. Early results show adding prebiotic fibers boosts its effect by 37%.
Fecal Microbiota Transplants
FMTs are approved for C. diff but are still being tested for autoimmune diseases. Researchers use special protocols to study how donor microbes help with conditions like lupus and rheumatoid arthritis.
Current FDA Approval Status
Studies are working on better donor screening and dosage. Six Phase II studies are looking at how FMTs affect multiple sclerosis patients. Results are expected by late 2024.
“Personalized microbial therapies could become first-line interventions within this decade,” notes lead researcher Dr. Alicia Tan in Nature Immunology’s 2023 year-end review.
These new approaches show how important your microbiome is in fighting autoimmune diseases. They offer hope beyond traditional treatments.
Implementing Changes Safely
Changing your gut ecosystem needs more than just wanting to help. It requires a careful plan and the help of experts. While it’s great to want to heal, trying too much on your own can harm your gut health and autoimmunity efforts. Here’s how to do it right.
Working With Functional Medicine
Functional medicine doctors are like detectives, looking for the real causes of problems. They spend a lot of time during your first visit, going over your health history.
Finding Qualified Practitioners
Search for doctors who are certified by the Institute for Functional Medicine (IFM) and know a lot about autoimmune diseases. Check their credentials on:
- State medical board licenses
- IFM’s official provider directory
- Patient reviews that talk about success with gut health
Make sure they know how to read stool tests and create plans just for you. Stay away from doctors who offer the same thing to everyone or suggest untested treatments like DIY fecal transplants.
Monitoring Progress
Keeping track of how you’re doing with gut health and autoimmunity is more than just keeping a journal. Lab tests give you real information about what’s going on inside you.
Key Biomarkers to Track Monthly
Focus on these three tests during your healing journey:
- Comprehensive Digestive Stool Analysis (CDSA): Shows how your gut bacteria are doing, inflammation levels, and how well you digest food
- LPS Antibodies: Checks how your immune system reacts to toxins from your gut
- Vitamin D3 Levels: Important for keeping your immune system in check and fixing your gut lining
Most doctors say to test these things every 8-12 weeks at first. Seeing these markers get better often means you’ll start to feel better in 3-6 months.
Healing your gut health and autoimmunity is like training for a marathon, not a sprint. Working with experts and keeping an eye on your progress helps you avoid big problems before they start.
Conclusion
New studies show a strong connection between gut health and autoimmune diseases. Dr. Martin Kriegel’s work on Enterococcus gallinarum found that gut bacteria can start inflammation in the body. This discovery, along with vaccine research, shows how important the microbiome is in causing autoimmune diseases.
Your gut lining is like a shield and a messenger. It helps control how your immune system reacts. This happens through molecular mimicry and cytokine signaling.
First, learn about your own microbiome. Doctors suggest getting a stool analysis from places like Genova Diagnostics or Diagnostic Solutions. Then, make diet changes, like avoiding gluten or dairy. Also, try stress-reducing activities like yoga or using apps for breathing exercises.
Getting help from a doctor is key when dealing with gut and autoimmune issues. Functional medicine doctors use tests from Cyrex Laboratories to make plans just for you. New medicines are being made, focusing on postbiotics and refined FMT that target specific bacteria.
As we learn more about gut health and autoimmune diseases, taking care of your microbiome is vital. Keep up with the latest research through the American Autoimmune Related Diseases Association. Your choices, like eating fermented foods or getting enough sleep, affect your health.