Did you know nearly 90 million Americans experience occasional nighttime disruptions? While many dismiss it as harmless, persistent noise from the throat could indicate deeper concerns. Vibrations in the airway often point to tissue obstruction, creating more than just an annoyance for bed partners.
Dr. Skiba explains, “Snoring stems from relaxed throat tissues during sleep.” This common issue affects up to half of adults, with higher risks for middle-aged men and postmenopausal women. Excess weight and poor sleep habits can worsen the problem.
Not all cases are equal. Occasional noise differs from obstructive sleep apnea (OSA), where breathing stops repeatedly. Both strain cardiovascular health over time. Recognizing the difference helps you take action before complications arise.
Key Takeaways
- Affects 25-50% of adults, with 90 million U.S. cases
- Indicates potential airway blockage or tissue vibration
- Higher risk for specific age and weight groups
- May signal OSA, linked to heart health concerns
- Professional diagnosis determines severity
Understanding the Science Behind Snoring
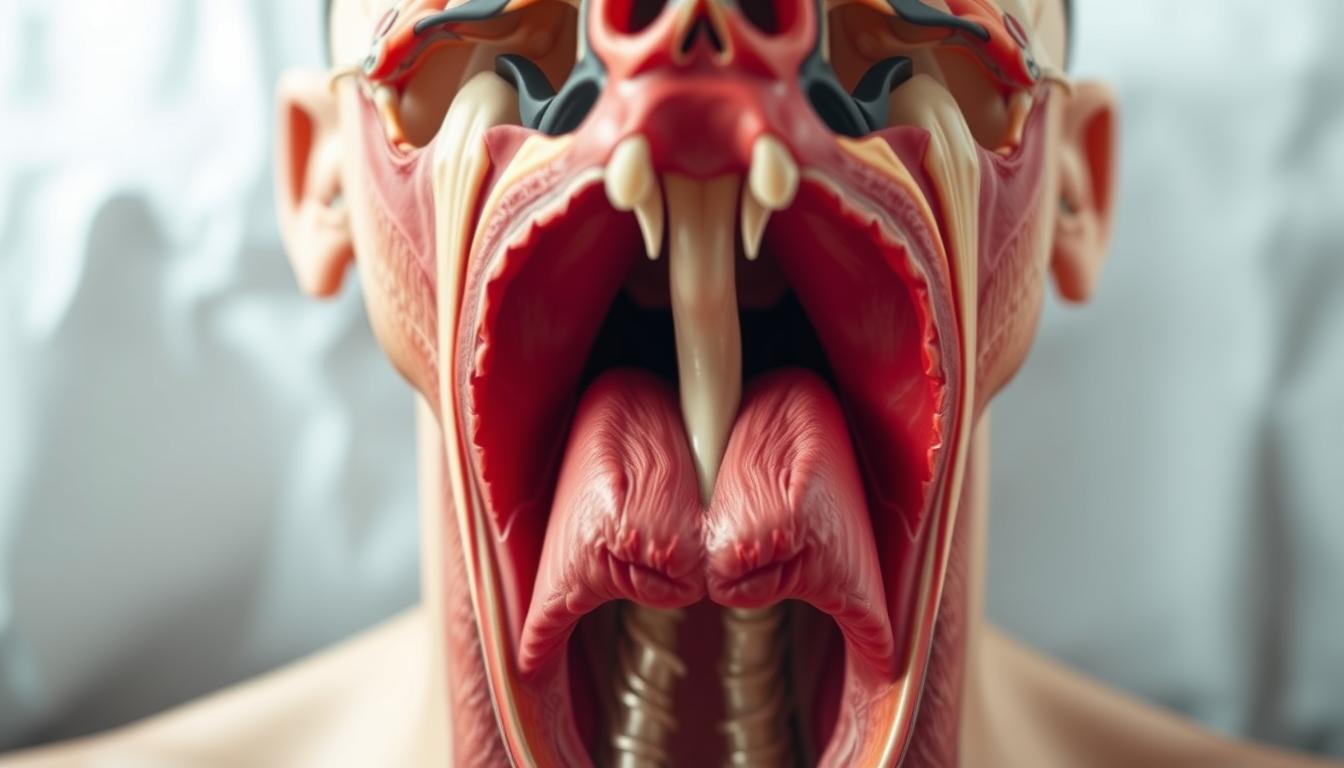
Behind every snore lies a complex interaction of muscles and airflow. When you sleep, relaxed tissues in your throat vibrate as air passes through, creating that familiar rumbling sound. “Snoring occurs when throat tissues vibrate during inhalation,” explains Dr. Skiba.
How Throat Tissue Vibrations Create Snoring Sounds
The soft palate and uvula—the fleshy areas at the back of your mouth—are key players. As you inhale, turbulent airflow causes these tissues to flutter, much like a flag in the wind. The narrower your airway, the louder the sound.
Anatomical factors amplify the issue. Enlarged tonsils, a deviated septum, or nasal congestion restrict space, forcing air to move faster. Gravity worsens it when you sleep on your back, as Dr. Skiba notes.
The Role of Airway Obstruction and Relaxed Muscles
Partial blockages lead to snoring; complete pauses signal sleep apnea. Alcohol and sedatives relax throat muscles further, increasing vibration intensity. Excess weight adds pressure, narrowing the throat’s passage.
Recognizing these mechanics helps distinguish harmless snoring from conditions like OSA. If your nighttime noises come with gasping or fatigue, consult a specialist.
What Snoring Says About Your Health—Beyond Just Noise
Many dismiss nighttime noise as harmless, but it could signal deeper health concerns. While occasional snoring is common, chronic cases may indicate obstructive sleep apnea (OSA)—a condition linked to serious complications.

Primary Snoring vs. Obstructive Sleep Apnea
Primary snoring is often benign, caused by relaxed throat tissues. However, OSA involves repeated breathing pauses, depriving your body of oxygen. “Untreated OSA accelerates cognitive decline and low testosterone,” warns Dr. Skiba.
Key differences:
| Factor | Primary Snoring | OSA |
|---|---|---|
| Breathing Interruptions | None | Frequent pauses |
| Health Impact | Minimal | High heart risk |
| Prevalence | 37 million Americans | 50% of loud snorers (JAMA) |
Cardiovascular Risks and Blood Pressure
OSA strains your heart by causing sudden oxygen drops. Studies link it to high blood pressure, stroke, and heart attacks. Even non-OSA snoring may elevate blood pressure due to disrupted sleep.
Overweight individuals face higher risks, as excess weight narrows airways. Weight management can significantly reduce severity.
“OSA increases hypertension risks by 40%—early diagnosis saves lives.”
When Snoring Signals a Serious Condition
Persistent snoring often masks underlying conditions requiring medical attention. While occasional noise is common, frequent episodes with gasping or fatigue may point to sleep apnea. Left untreated, this disorder strains your heart and reduces oxygen levels.

Recognizing Red Flags
Key symptoms of obstructive sleep apnea (OSA) include:
- Choking or gasping during night
- Morning headaches and irritability
- Partner-reported pauses in breathing
Dr. Skiba warns, “High blood pressure or heart disease? Get tested for OSA.” Untreated cases may shorten life expectancy by 10–15 years (AMA).
Why Some Face Higher Risks
Men and overweight people are more prone to OSA. Biological factors like narrower airways and fatty throat tissue increase risk. Hormonal changes during menopause also relax airway muscles.
| Group | Risk Factor | Prevention Tip |
|---|---|---|
| Men | Anatomical airway narrowing | Sleep on your side |
| Overweight individuals | Fat compresses the throat | Lose 10% of body weight |
| Postmenopausal women | Reduced muscle tone | Consult a sleep specialist |
If you stop breathing repeatedly at night, seek evaluation. Early diagnosis can prevent cardiovascular damage.
How Doctors Diagnose Snoring-Related Disorders
Diagnosing sleep-related breathing issues requires precise medical evaluation. Specialists use two main methods: home tests and in-lab sleep studies. Each has distinct advantages, but accuracy varies.
Home Sleep Tests vs. In-Lab Sleep Studies
Home tests are convenient, measuring breathing patterns and oxygen levels overnight. However, they miss 30% of mild-to-moderate obstructive sleep apnea cases (AMA). For definitive results, in-lab polysomnography remains the gold standard.
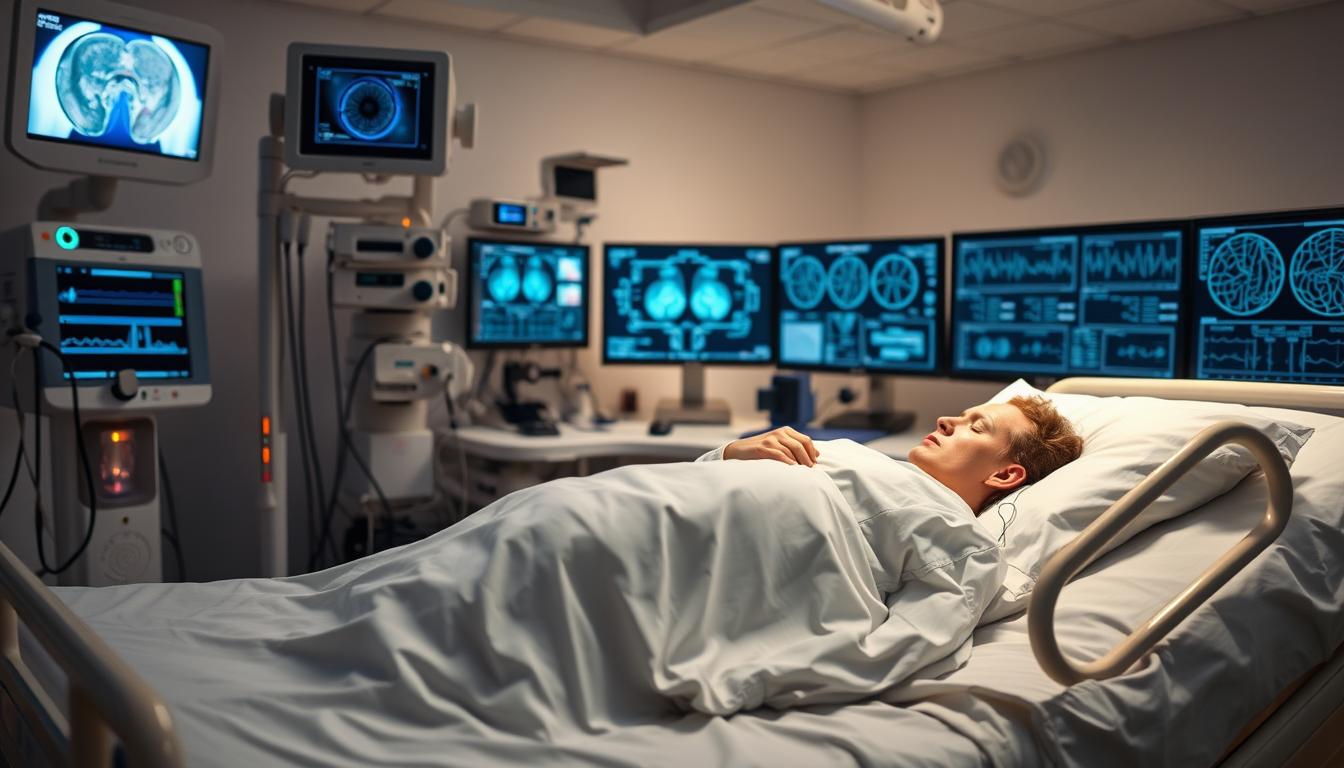
In-lab studies track brain waves, heart rate, and air flow. Dr. Skiba notes, “They capture subtle disruptions home tests might overlook.” A “split-night” study can diagnose OSA and calibrate CPAP therapy in one session.
Why Follow-Up Testing Matters for Accuracy
Negative home tests often require in-lab confirmation. Pulse oximetry and airflow sensors help identify partial blockages. UC Health’s advanced assessments combine both methods for reliability.
- Home tests: Portable but less detailed.
- In-lab studies: Comprehensive, monitoring 16+ metrics.
- Split-night studies: Efficient for severe cases.
“Always follow negative home tests with in-lab studies—OSA hides in plain sight.”
Immediate Adjustments to Reduce Snoring
Simple nighttime tweaks can quiet disruptive snoring and improve rest. Minor changes to sleep position or bedroom setup often yield significant results. Start with these evidence-backed strategies.
The Benefits of Side Sleeping and Elevated Positioning
Sleeping on your back worsens snoring by letting the tongue collapse into the throat. A Kaiser Permanente study found side sleeping cuts episodes by 50%. Try a tennis ball sewn into pajamas or vibrating belts to train yourself.

Elevating your head 30 degrees eases airflow. Use wedge pillows or bed risers. “Gravity pulls tissues downward—elevation counteracts this,” notes Dr. Becker. For persistent nasal congestion, UC Health’s ENT program assesses structural issues.
Mouth Taping and Nasal Strips: Do They Work?
Nasal strips widen nostrils, improving sleep quality twofold versus placebos. They’re ideal for mild cases or allergy-related snoring. Mouth taping, however, is controversial. It may help mouth breathers but risks harm if sleep apnea is present.
“Treat allergies or a deviated septum first—taping is a last resort.”
For quick relief, combine these methods. Address root causes like weight or alcohol use for long-term results.
Medical Treatments for Chronic Snoring
Modern medicine provides targeted solutions for persistent snoring that resists home remedies. When lifestyle changes prove insufficient, clinical treatments address anatomical causes with precision. Options range from non-invasive devices to surgical interventions, each targeting specific airway issues.
Oral Appliances and CPAP Machines
Dentist-fitted oral appliances reposition the jaw to prevent throat tissue collapse. Mandibular advancement devices, the most common type, reduce snoring in 60% of users by gently moving the lower jaw forward. These custom devices are ideal for mild-to-moderate obstructive sleep apnea.
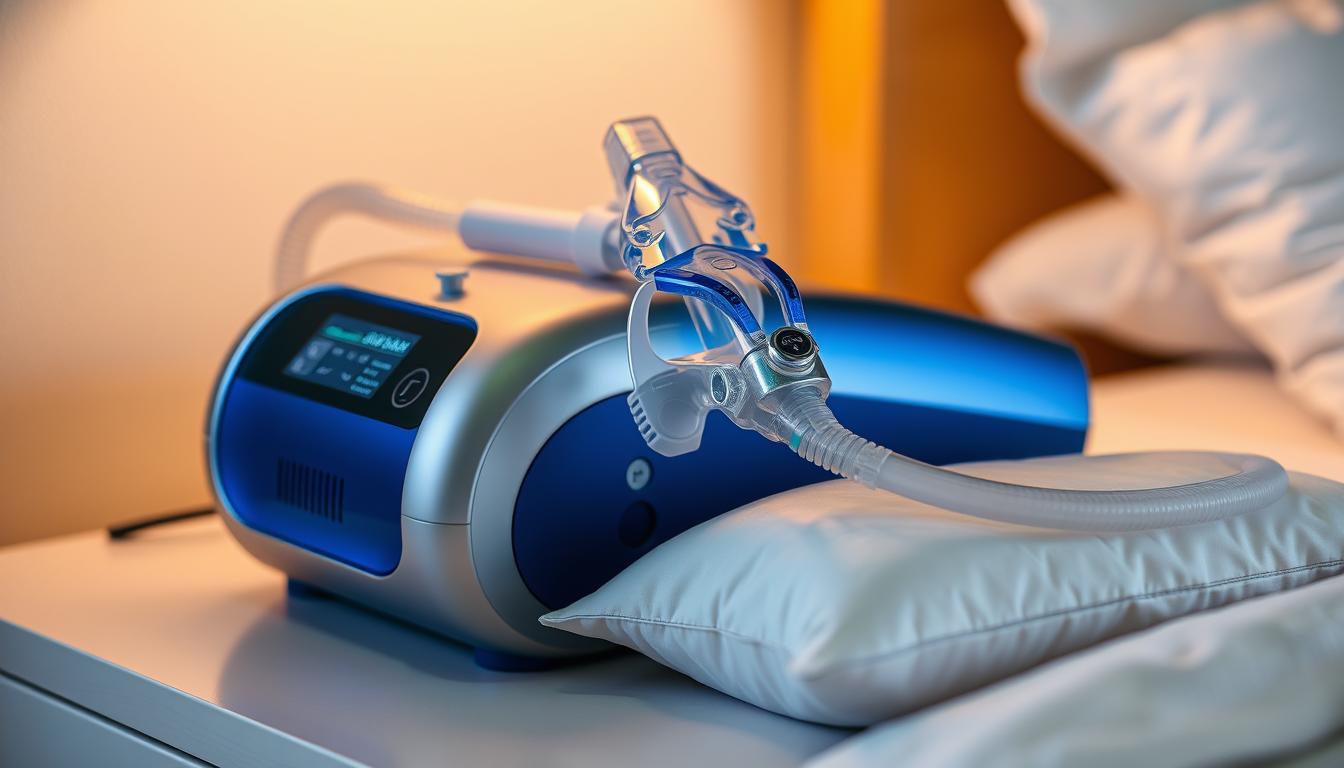
CPAP (continuous positive airway pressure) machines deliver pressurized air through a mask, acting as a pneumatic splint for airways. “CPAP is the frontline treatment for OSA-related snoring,” emphasizes Dr. Skiba. The American Medical Association reports 80% effectiveness in reducing snoring among apnea patients.
Surgical Options for Lasting Relief
When devices aren’t viable, surgery modifies airway anatomy. Laser-assisted uvulopalatoplasty (LAUP) reshapes the soft palate, with 2-3 week recovery periods. Pillar implants—tiny inserts that stiffen floppy tissues—reduce snoring frequency by 60% according to clinical studies.
| Treatment | Best For | Effectiveness |
|---|---|---|
| Oral Appliances | Mild apnea, primary snoring | 60% reduction |
| CPAP | Moderate-severe obstructive sleep apnea | 80% reduction |
| Pillar Implants | Palatal flutter snoring | 60% reduction |
Insurance typically covers only apnea-related treatments. Snoring-only procedures like LAUP often require out-of-pocket payment. Consult a specialist to match your anatomy with the optimal intervention.
Lifestyle Changes to Address Root Causes
Your daily habits play a surprising role in nighttime breathing patterns. While devices and surgeries offer solutions, modifying key behaviors often resolves snoring at its source. Two factors—weight management and substance avoidance—deliver measurable improvements.
How Weight Affects Airway Function
Excess body weight directly impacts breathing by compressing throat tissues. Kaiser Permanente research shows losing 10% of your weight reduces snoring frequency by 30%. Those with a BMI over 30 face higher risks due to fatty deposits narrowing the airway.
For sustainable results, combine Mediterranean diet principles with aerobic exercise. “Even modest weight loss improves sleep quality by reducing tissue vibration,” notes Dr. Becker. Target 150 weekly minutes of brisk walking or swimming to strengthen respiratory muscles.
The Hidden Impact of Alcohol and Sedatives
Drinking within four hours of bedtime relaxes throat muscles excessively. Studies confirm moderate alcohol consumption triples snoring intensity by weakening tissue tension. Sedatives like benzodiazepines and opioids worsen this effect.
- Avoid nightcaps—opt for herbal tea instead
- Discuss sedative alternatives with your doctor
- Quit smoking to reduce pharyngeal inflammation
These adjustments complement medical treatments for lasting health benefits. Small, consistent changes often yield the most significant improvements in nighttime breathing.
Conclusion: Taking Action for Better Sleep and Health
Nighttime noise might seem harmless, but it often reflects deeper concerns. Chronic snoring can signal airway blockages or sleep disorders like OSA. If you experience fatigue or gasping, a doctor can help.
For severe cases, UC Health offers advanced solutions like hypoglossal nerve stimulators. These devices gently keep airways open during sleep, reducing risks tied to the condition.
“Don’t ignore snoring—it’s treatable,” urges Dr. Skiba. Early intervention protects your health over time. Call UC Health at 513-475-8400 for a consultation today.